What is Liver Cirrhosis?
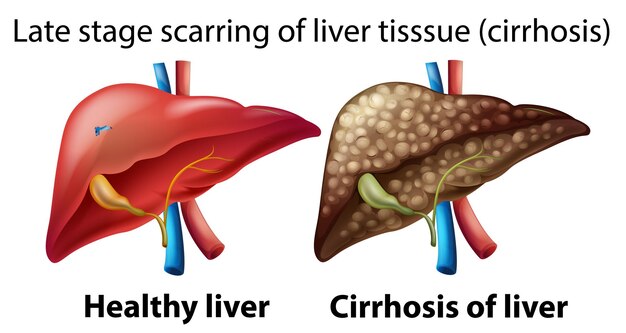
Liver cirrhosis is a chronic liver disease characterized by the gradual destruction and scarring of liver tissue, which impairs the liver’s ability to function properly. This progressive condition often develops over many years and can lead to severe complications, including liver failure, internal bleeding, and liver cancer. Cirrhosis is the final stage of many liver diseases and can result from various causes such as long-term alcohol abuse, viral hepatitis, or fatty liver disease.
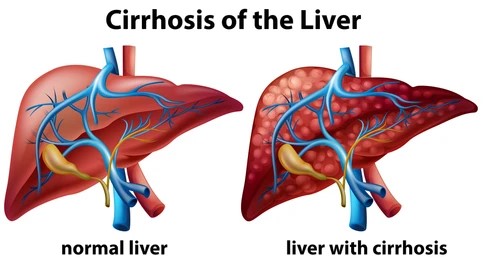
Types of Liver Cirrhosis?
Cirrhosis can be classified based on its cause or the extent of damage. The primary types include:
- Alcoholic Cirrhosis: Resulting from chronic alcohol consumption, leading to liver damage.
- Chronic Hepatitis Cirrhosis: Caused by long-standing hepatitis infections, particularly hepatitis B and hepatitis C.
- Non-Alcoholic Fatty Liver Disease (NAFLD): Cirrhosis caused by fat accumulation in the liver, not related to alcohol consumption.
- Biliary Cirrhosis: Caused by a blockage in the bile ducts, which can lead to bile buildup and liver damage.
- Hemochromatosis: An inherited condition where excess iron is deposited in the liver, leading to cirrhosis.
- Wilson’s Disease: A genetic disorder that results in excess copper in the liver, leading to cirrhosis.
- Autoimmune Hepatitis: A condition where the body’s immune system attacks the liver, leading to inflammation and scarring.
Causes of Liver Cirrhosis?
The main causes of liver cirrhosis include:
- Chronic alcohol use: Heavy and prolonged alcohol consumption is one of the most common causes of cirrhosis.
- Hepatitis B and C: Chronic infections with these viruses can lead to liver damage, cirrhosis, and liver cancer.
- Fatty liver disease: Conditions like non-alcoholic fatty liver disease (NAFLD) or non-alcoholic steatohepatitis (NASH) can lead to cirrhosis when the fat accumulation in the liver is not managed.
- Chronic bile duct problems: Conditions such as primary biliary cirrhosis (PBC) and primary sclerosing cholangitis (PSC) can cause damage to the bile ducts, leading to cirrhosis.
- Genetic disorders: Diseases like hemochromatosis (iron overload) and Wilson’s disease (copper accumulation) can result in cirrhosis.
- Medications and toxins: Long-term use of certain medications or exposure to harmful substances can also contribute to liver cirrhosis.
Symptoms of Liver Cirrhosis?
In the early stages, cirrhosis may have no obvious symptoms. As the liver becomes more damaged, however, a person may experience:
- Fatigue and weakness: Feeling constantly tired and weak, even with adequate rest.
- Unexplained weight loss: Losing weight without trying, which may be accompanied by muscle loss.
- Nausea and vomiting: Ongoing nausea or vomiting, especially after eating.
- Jaundice: Yellowing of the skin and eyes, often a sign that the liver can no longer process bilirubin effectively.
- Swelling: Swelling in the abdomen (ascites) or legs (edema) due to fluid buildup.
- Itchy skin: Persistent itching, often due to bile salts accumulating in the skin.
- Easy bruising and bleeding: Bleeding more easily than normal, such as nosebleeds or bruises, due to reduced clotting factor production by the liver.
- Confusion or difficulty thinking: Hepatic encephalopathy can cause confusion, forgetfulness, and difficulty concentrating due to the buildup of toxins in the brain.
Diagnosis of Liver Cirrhosis?
The diagnosis of cirrhosis involves a combination of medical history, physical examination, and diagnostic tests:
- Blood tests: These include liver function tests to check for elevated levels of liver enzymes, bilirubin, and clotting factors. The liver biopsy may be done to confirm the presence of cirrhosis.
- Imaging tests:
- Ultrasound: Helps to visualize liver abnormalities, such as changes in size or texture.
- CT scan and MRI: Used to examine the liver in greater detail, particularly to check for tumors, fluid buildup, and other complications.
- Elastography: Measures liver stiffness and is a non-invasive way to assess the extent of fibrosis (scarring).
- Endoscopy: Used to check for complications of cirrhosis, such as varices (enlarged veins in the esophagus) that can lead to bleeding.
- Liver biopsy: In some cases, a liver biopsy may be performed to confirm the diagnosis and determine the extent of liver damage.
Treatment and Management of Liver Cirrhosis?
Treatment for liver cirrhosis aims to manage symptoms, prevent complications, and slow the progression of liver damage. Key treatment options include:
- Lifestyle changes:
- Avoid alcohol: The most critical change for those with alcoholic cirrhosis.
- Healthy diet: A balanced diet, low in salt and high in nutrients, helps manage symptoms like swelling and fatigue.
- Weight management: Maintaining a healthy weight is crucial, particularly for those with NAFLD or NASH.
- Medications:
- Diuretics: These may be prescribed to help reduce fluid buildup in the abdomen (ascites) or legs (edema).
- Beta-blockers: Used to lower blood pressure in the portal vein and prevent complications like varices (enlarged veins).
- Antiviral medications: For patients with hepatitis B or C, antiviral treatment can reduce liver inflammation and damage.
- Lactulose: This medication helps reduce the buildup of toxins in the brain and can treat hepatic encephalopathy.
- Management of complications:
- Endoscopy or surgery for variceal bleeding: If cirrhosis causes varices in the esophagus or stomach, endoscopic treatment or surgery may be necessary.
- Liver transplant: In severe cases where liver failure occurs, a liver transplant may be the only option. This is typically considered when the liver can no longer perform its essential functions.
Complications of Liver Cirrhosis?
Cirrhosis can lead to several complications, including:
- Liver failure: In the advanced stages, cirrhosis can result in the liver’s inability to perform vital functions, such as detoxifying the blood or producing proteins.
- Portal hypertension: Increased blood pressure in the portal vein can lead to the development of varices and ascites.
- Hepatocellular carcinoma (liver cancer): Cirrhosis significantly increases the risk of developing liver cancer.
- Hepatic encephalopathy: A build-up of toxins, especially ammonia, in the bloodstream that can affect brain function and cause confusion, coma, and even death.
- Kidney failure: Cirrhosis can also affect kidney function, leading to a condition called hepatorenal syndrome.
- Infections: People with cirrhosis are at higher risk of infections, particularly spontaneous bacterial peritonitis (SBP), a severe infection of the abdominal fluid.
Prevention of Liver Cirrhosis?
While cirrhosis is often preventable, especially when caught early, the following steps can reduce the risk:
- Avoid excessive alcohol use: Limiting alcohol intake helps prevent alcoholic liver disease, which is a leading cause of cirrhosis.
- Vaccination against hepatitis: Getting vaccinated for hepatitis B and seeking treatment for hepatitis C can prevent cirrhosis caused by viral infections.
- Maintain a healthy weight: Controlling body weight and managing conditions like diabetes can help prevent fatty liver disease and NASH.
- Avoiding toxins and drugs: Reducing exposure to harmful substances and not overusing medications that can harm the liver, such as certain painkillers and supplements.
When to See a Doctor?
You should see a doctor if you experience symptoms such as fatigue, unexplained weight loss, jaundice, or swelling in the abdomen or legs. If you have risk factors like chronic alcohol use, viral hepatitis, or obesity, regular check-ups with a healthcare provider are essential to monitor liver health.


