What is Hypomelanosis of Ito?
Hypomelanosis of Ito is a rare neurocutaneous disorder primarily characterized by streaks or swirls of lighter-colored skin (hypopigmentation) that follow the lines of Blaschko—natural patterns of skin development. These skin changes are often present at birth or appear early in childhood and are sometimes accompanied by neurological, skeletal, or developmental abnormalities.
It is not a single disease but rather a syndrome that can affect multiple systems in the body.

What causes Hypomelanosis of Ito?
The exact cause is not always clear. However, Hypomelanosis of Ito is believed to result from genetic mosaicism—a condition where some cells in the body have different genetic makeup due to a mutation occurring early in development.
In most cases, the condition is not inherited but occurs as a sporadic mutation. Rarely, it may follow mosaic autosomal dominant inheritance if passed on from a parent with mosaicism.
Who is at risk?
- Both males and females can be affected, though it is more commonly reported in females.
- The condition usually appears in infancy or early childhood.
- There is no known specific environmental or lifestyle risk factor.
What are the symptoms of Hypomelanosis of Ito?
Skin Symptoms:
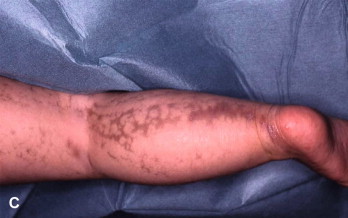
- Swirled, streaked, or linear patches of lighter skin
- Patterns follow the lines of Blaschko
- Hypopigmentation may appear on the trunk, limbs, face, or scalp
- These patches do not cause itching, pain, or scaling
Other Possible Symptoms (Not always present):
Around half of individuals may have additional complications, such as:
Neurological:
- Developmental delays
- Intellectual disability
- Seizures or epilepsy
- Muscle weakness or abnormal muscle tone
Skeletal:
- Scoliosis (curved spine)
- Limb length differences
- Abnormalities in fingers or toes
Eye and Dental:
- Strabismus (crossed eyes)
- Refractive errors
- Dental anomalies (missing or abnormally shaped teeth)
Because the symptoms vary so widely, each person’s experience with Hypomelanosis of Ito can be very different.
How is Hypomelanosis of Ito diagnosed?
Diagnosis is based on a combination of:
- Physical examination, especially observation of skin patterns
- Medical and developmental history
- Neurological and developmental assessments
- Skin biopsy (rarely done) to rule out other causes of hypopigmentation
- Genetic testing or chromosomal studies to detect mosaicism or other genetic abnormalities
A diagnosis is often made clinically (based on signs and symptoms), particularly when other features are present along with the skin changes.
How is Hypomelanosis of Ito treated?
There is no cure for the condition itself, but treatment focuses on managing individual symptoms. A multidisciplinary team approach is often needed, depending on the systems involved.
Management may include:
- Regular developmental monitoring
- Speech, physical, and occupational therapy
- Antiepileptic medications for seizures
- Orthopedic care for skeletal issues
- Vision and dental care
- Educational support and individualized learning plans
Skin discoloration usually does not require treatment, although sun protection may be advised for sensitive areas.
What are the complications of Hypomelanosis of Ito?
Potential complications vary depending on the severity of associated abnormalities:
- Learning difficulties
- Motor development delays
- Seizure disorders
- Orthopedic deformities
- Vision or hearing issues
Not every person with Hypomelanosis of Ito will have complications. Some may have only the skin findings with no other health concerns.
What is the outlook for people with Hypomelanosis of Ito?
The prognosis depends on the extent and severity of associated neurological or systemic issues. Individuals with only skin involvement usually have a normal life expectancy and development. When additional complications are present, early intervention can greatly improve quality of life and developmental outcomes.
Can Hypomelanosis of Ito be prevented?
- It cannot be prevented as it usually arises from a spontaneous mutation during early development.
- Genetic counseling may be offered to families when mosaicism or a genetic abnormality is detected.
- Early diagnosis and support are key in managing symptoms and improving outcomes.


