What Is Insulin Allergy?
Insulin allergy is a rare allergic reaction to insulin injections, typically seen in people with diabetes who use insulin to control blood sugar levels. The reaction may be to the insulin molecule itself, or to additives in the formulation such as preservatives (zinc, protamine, or meta-cresol).
Although insulin is a life-saving treatment for many, allergic reactions can range from mild skin irritation to severe systemic responses.

How Common Is Insulin Allergy?
Insulin allergy is considered uncommon, especially since the introduction of human recombinant insulin, which is much less likely to cause allergic reactions compared to older animal-derived insulin. It affects less than 2% of insulin users.
What Causes Insulin Allergy?
Insulin allergy can be caused by:
- The insulin molecule itself (rare, more common with animal-based insulin)
- Additives or preservatives in insulin preparations
- Contaminants or improper injection technique
- Immune system sensitivity to injected proteins
Risk factors include:
- Previous allergic reactions
- Multiple insulin formulations
- Autoimmune conditions
- Frequent switching of insulin brands or types
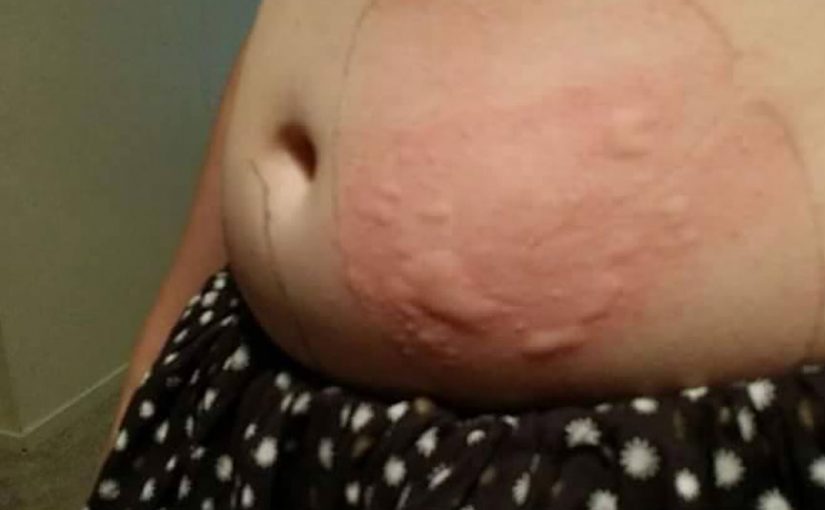
What Are the Symptoms of Insulin Allergy?
Symptoms usually appear shortly after insulin injection and can vary from mild to severe:
Local Reactions:
- Redness, swelling, or itching at the injection site
- Skin rash or hives
- Warmth or pain at the site
Systemic Reactions:
- Generalized rash or hives
- Shortness of breath or wheezing
- Nausea or vomiting
- Rapid heartbeat
- Anaphylaxis (life-threatening reaction with airway swelling and low blood pressure)
In some cases, the symptoms can develop hours after injection and might be delayed or misdiagnosed.
How Is Insulin Allergy Diagnosed?
Diagnosis is based on medical history, symptoms, and sometimes allergy testing. Tests may include:
- Skin prick or intradermal testing using different insulin preparations
- Blood tests for IgE antibodies specific to insulin
- Injection site biopsy (in chronic or unusual cases)
- Reviewing response to changes in insulin type or additives
Consultation with an allergist or immunologist may be necessary for complex cases.
How Is Insulin Allergy Treated?
Treatment depends on the type and severity of the reaction.
Mild Reactions:
- Antihistamines to relieve itching or swelling
- Topical steroids for injection-site reactions
- Changing insulin brands or switching to a form without the triggering additive
Moderate to Severe Reactions:
- Desensitization protocols: Gradual reintroduction of insulin under medical supervision
- Use of insulin analogs with fewer allergic components
- Insulin pumps (to provide smaller, continuous doses)
- Premedication with antihistamines or corticosteroids before injection
Emergency Treatment:
- Epinephrine (adrenaline) for anaphylaxis
- Emergency room care for airway or cardiovascular symptoms
It’s important that all people with insulin allergy wear medical ID and have an emergency action plan in place.
Can Insulin Allergy Be Prevented?
While it can’t always be prevented, you can reduce the risk by:
- Using modern human or analog insulin (less allergenic)
- Avoiding frequent switching of insulin brands
- Practicing clean and proper injection techniques
- Not reusing needles
- Rotating injection sites
- Being cautious if you have a history of drug allergies
Always inform your healthcare provider if you’ve had previous allergic reactions to any medications.
When Should You Seek Medical Help?
You should seek medical attention if you experience:
- Worsening skin reactions after insulin use
- Hives or itching all over the body
- Swelling of the face, lips, or throat
- Difficulty breathing or dizziness
- Any signs of anaphylaxis
Prompt diagnosis and management are essential to prevent complications.
What’s the Outlook for People With Insulin Allergy?
With proper medical support and careful insulin management, most people can continue using insulin safely. Many cases can be managed through allergy-friendly insulin options, desensitization, or insulin pumps.
In very rare cases, doctors may recommend non-insulin medications or pancreas/islet cell transplants, but these are typically reserved for extreme situations.


