What Is Exocrine Pancreatic Insufficiency?
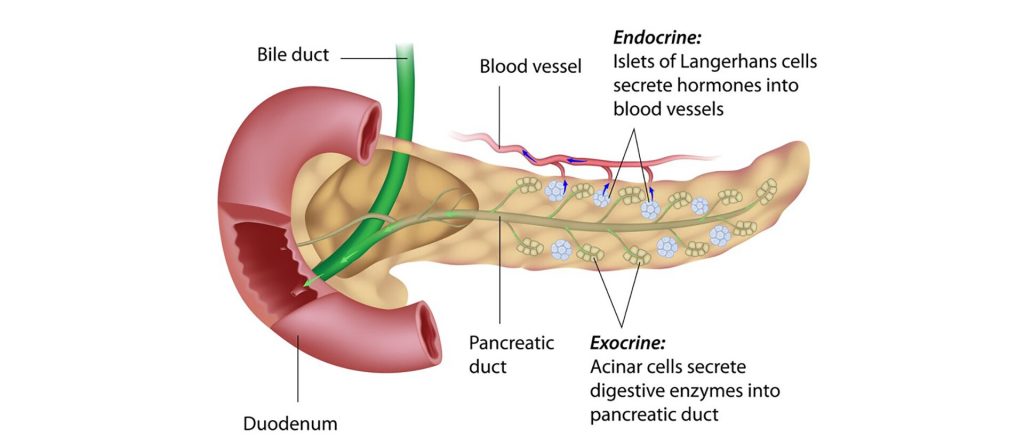
Exocrine Pancreatic Insufficiency (EPI) is a condition in which the pancreas does not produce enough digestive enzymes to properly break down food in the small intestine. These enzymes—lipase (for fats), amylase (for carbohydrates), and protease (for proteins)—are essential for nutrient absorption. Without them, the body struggles to digest food, leading to malnutrition, weight loss, and digestive symptoms.
EPI can affect both children and adults and is commonly associated with other underlying health conditions.
What Causes Exocrine Pancreatic Insufficiency?
EPI is usually the result of damage to the pancreas or a disease that affects its function. Common causes include:
- Chronic pancreatitis: Long-term inflammation of the pancreas can damage the cells that produce digestive enzymes.
- Cystic fibrosis: A genetic disorder that leads to thick mucus buildup, blocking enzyme flow.
- Pancreatic cancer: Tumors can interfere with the production or release of enzymes.
- Diabetes: Especially type 1, where long-standing diabetes can impair pancreatic function.
- Celiac disease: Damage to the intestine may affect enzyme activation.
- Crohn’s disease: Inflammation in the digestive tract may impair absorption and pancreatic function.
- Surgical removal of the pancreas or stomach: May limit or eliminate enzyme production.
In some cases, the cause of EPI remains unclear (idiopathic EPI).
What Are the Symptoms of Exocrine Pancreatic Insufficiency?
The symptoms of EPI typically relate to poor digestion and nutrient absorption. These can include:
- Chronic diarrhea
- Steatorrhea (fatty, oily, or foul-smelling stools)
- Unintended weight loss
- Bloating and gas
- Abdominal pain or discomfort
- Vitamin deficiencies (A, D, E, K)
- Fatigue or weakness
- Poor growth in children
Because many of these symptoms overlap with other digestive conditions, EPI is often misdiagnosed or delayed in diagnosis.

How Is Exocrine Pancreatic Insufficiency Diagnosed?
Diagnosing EPI involves evaluating digestive symptoms and testing for enzyme levels and nutrient absorption. Common methods include:
- Stool tests: To check for undigested fat (steatorrhea) or low levels of pancreatic elastase.
- Blood tests: To detect vitamin deficiencies or malnutrition.
- Breath tests: To assess fat digestion and absorption.
- Imaging tests: Such as CT scans, MRI, or endoscopic ultrasound to evaluate the pancreas.
- Trial of enzyme therapy: Improvement of symptoms with enzyme supplementation can confirm the diagnosis.
How Is Exocrine Pancreatic Insufficiency Treated?
EPI is a manageable condition with proper treatment. The main goal is to replace the missing enzymes and ensure adequate nutrition. Common treatments include:
- Pancreatic enzyme replacement therapy (PERT): Prescription enzyme capsules taken with meals help digest food effectively. Examples include pancrelipase products (Creon, Zenpep, Pancreaze).
- Dietary changes:
- Eating smaller, frequent meals.
- Following a balanced diet rich in nutrients.
- Limiting high-fat foods if they worsen symptoms.
- Vitamin supplementation: Especially fat-soluble vitamins A, D, E, and K.
- Management of underlying conditions: Such as treating pancreatitis or celiac disease if present.
- Regular follow-ups: Monitoring symptoms and nutritional status over time.
What Is the Outlook for People With EPI?
With early diagnosis and proper treatment, people with EPI can manage their symptoms effectively and maintain a good quality of life. However, untreated EPI can lead to:
- Malnutrition and vitamin deficiencies
- Weight loss and muscle wasting
- Bone thinning (osteoporosis or osteopenia)
- Poor growth and development in children
- Weakened immune function
Lifelong enzyme therapy and proper dietary guidance are often necessary for long-term control.
When Should You See a Doctor?
You should consult a healthcare provider if you notice:
- Ongoing diarrhea or oily stools
- Significant weight loss without trying
- Frequent bloating, gas, or abdominal pain
- Symptoms of vitamin deficiency (vision problems, bone pain, fatigue)
- Difficulty gaining weight or growing in children
Early evaluation can lead to quicker relief and better long-term outcomes.
Can Exocrine Pancreatic Insufficiency Be Prevented?
While EPI itself cannot always be prevented, reducing risk factors for pancreatic damage may help. These include:
- Avoiding excessive alcohol consumption
- Managing conditions like diabetes or celiac disease
- Not smoking, as it increases the risk of pancreatic diseases
- Eating a healthy, balanced diet


