A serious and potentially life-threatening complication of diabetes
What is Diabetic Ketoacidosis?
Diabetic Ketoacidosis (DKA) is a medical emergency that occurs when the body cannot use glucose (sugar) properly due to insulin deficiency. Instead, it starts breaking down fat for energy, which produces ketones—acidic substances that accumulate in the blood and make it dangerously acidic.
DKA mainly affects people with type 1 diabetes, but it can also occur in those with type 2 diabetes, especially under stress, infection, or missed insulin doses.
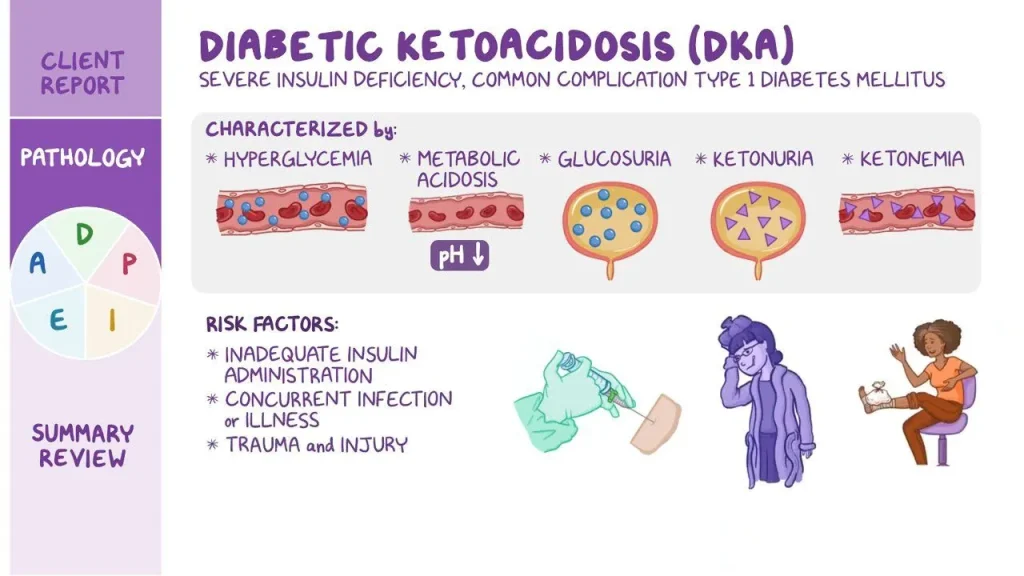
What causes Diabetic Ketoacidosis?
The main triggers of DKA include:
- Missed insulin injections or inadequate insulin therapy
- Infections (e.g., urinary tract infections, pneumonia)
- Undiagnosed diabetes
- Illnesses or stress (e.g., surgery, trauma, heart attack)
- Poorly managed blood sugar levels
- Certain medications (e.g., steroids, diuretics, or SGLT2 inhibitors)
When insulin is lacking, the body can’t use glucose, so it burns fat instead. This produces ketones, which accumulate and lead to metabolic acidosis—a life-threatening imbalance in blood chemistry.
Who is at risk?
- People with type 1 diabetes
- Those with type 2 diabetes under stress or illness
- Individuals who skip insulin doses
- People with poor glucose control
- Children or teens with new-onset diabetes
- Patients taking SGLT2 inhibitors
What are the symptoms?
Symptoms usually develop over a few hours and include:
- Extreme thirst and dry mouth
- Frequent urination
- High blood glucose levels
- Nausea and vomiting
- Abdominal pain
- Weakness or fatigue
- Rapid, deep breathing (Kussmaul respirations)
- Fruity or acetone-like breath odor
- Confusion, drowsiness, or unconsciousness (in severe cases)
What are the complications?
If not treated quickly, DKA can result in:
- Severe dehydration
- Electrolyte imbalances (especially potassium)
- Cerebral edema (brain swelling)—especially in children
- Shock
- Coma
- Death
How is it diagnosed?
Diagnosis is made through:
- Medical history and symptoms
- Blood tests:
- Elevated blood glucose (usually >250 mg/dL)
- High blood ketone levels
- Low blood pH (acidosis)
- Low bicarbonate levels
- Increased anion gap
- Urine tests for glucose and ketones
- Monitoring of electrolyte levels, especially potassium and sodium
How is it treated?
DKA requires hospitalization and urgent treatment, including:
- Intravenous fluids to correct dehydration
- Insulin therapy to reduce blood glucose and stop ketone production
- Electrolyte replacement (especially potassium)
- Treatment of the underlying cause (e.g., infection)
- Monitoring of vital signs, blood sugar, and acid-base balance
Frequent blood tests and monitoring are essential to ensure safe recovery.
What is the prognosis?
- With prompt medical care, most people recover fully
- Delayed treatment can result in severe complications or death
- DKA can recur if diabetes is not well managed
Can Diabetic Ketoacidosis be prevented?
Yes, prevention includes:
- Strict adherence to insulin therapy
- Regular blood glucose monitoring
- Staying hydrated, especially during illness
- Recognizing early symptoms of DKA
- Having a diabetes management plan for sick days
- Seeking medical help early if blood sugar levels stay high


