What Is Intestinal Tuberculosis?
Intestinal tuberculosis (TB) is a form of extrapulmonary tuberculosis that affects the gastrointestinal tract, most commonly the ileocecal region (where the small and large intestines meet). It is caused by the bacteria Mycobacterium tuberculosis, the same organism that causes lung TB.
This condition can mimic other intestinal diseases like Crohn’s disease, making diagnosis challenging.
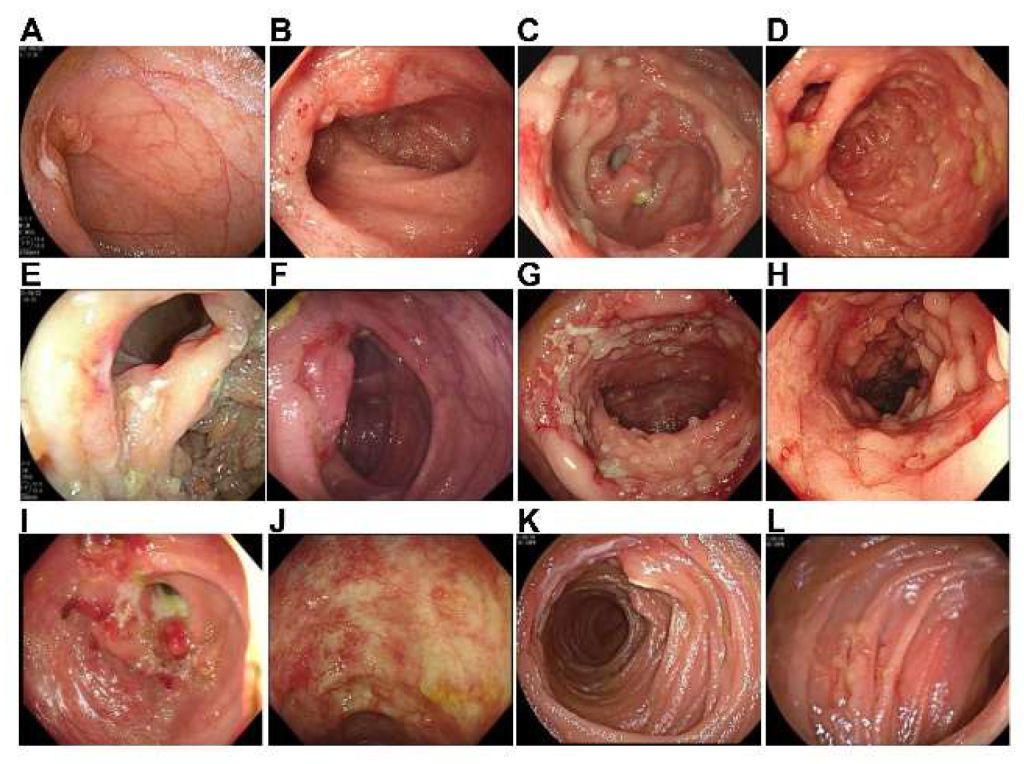
How Does Tuberculosis Reach the Intestines?
TB bacteria can reach the intestines through:
- Swallowing infected sputum from active pulmonary TB
- Hematogenous spread from other infected sites (like lungs or lymph nodes)
- Consumption of contaminated food (especially unpasteurized milk)
- Direct spread from adjacent organs
What Are the Symptoms of Intestinal Tuberculosis?
The symptoms are usually gradual and may include:
- Chronic abdominal pain, especially in the lower right side
- Weight loss
- Low-grade fever, especially in the evening
- Loss of appetite
- Diarrhea or constipation
- Abdominal swelling or masses
- Intestinal obstruction or perforation in advanced cases
- Occasionally, bloody stools
Symptoms can mimic other diseases like appendicitis, Crohn’s disease, or cancer.
How Is Intestinal Tuberculosis Diagnosed?
Diagnosis can be difficult due to nonspecific symptoms. Common tools include:
- Abdominal imaging (Ultrasound, CT scan) – may show thickened bowel walls or enlarged lymph nodes
- Colonoscopy – can visualize ulcers or narrowing and allows for biopsy
- Biopsy of intestinal tissue – to detect TB bacteria or granulomas
- Stool tests – to check for TB bacteria (though not always reliable)
- PCR or GeneXpert testing – for rapid TB diagnosis
- Tuberculin skin test (Mantoux) or IGRA blood test – to assess TB exposure
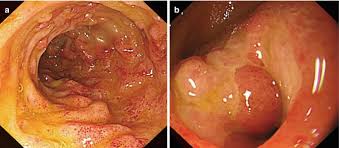
How Is Intestinal Tuberculosis Treated?
The cornerstone of treatment is anti-tubercular therapy (ATT), usually for 6 to 9 months, including:
- Isoniazid
- Rifampicin
- Pyrazinamide
- Ethambutol
Treatment phases include:
- Intensive phase (2 months) – 4 drugs
- Continuation phase (4–7 months) – usually 2 drugs
In some cases, surgery may be needed for:
- Intestinal obstruction
- Perforation
- Abscesses or fistulas
Can Intestinal Tuberculosis Be Cured?
Yes, with early diagnosis and proper treatment, intestinal TB can be fully cured. Delayed treatment, however, increases the risk of complications and surgical interventions.
Who Is at Risk for Intestinal Tuberculosis?
People at higher risk include:
- Individuals with active or past pulmonary TB
- Those living in or coming from TB-endemic areas
- Immunocompromised patients, including those with HIV/AIDS
- People with malnutrition
- Individuals on long-term steroids or chemotherapy
- Close contacts of TB patients
What Are the Complications of Intestinal TB?
If untreated or misdiagnosed, it may lead to:
- Chronic intestinal obstruction
- Intestinal perforation
- Abscess formation
- Malabsorption
- Strictures or fistulas
How Can Intestinal Tuberculosis Be Prevented?
Prevention strategies include:
- Early detection and treatment of pulmonary TB
- Avoiding unpasteurized dairy products
- Good hygiene and sanitation practices
- BCG vaccination in countries with high TB prevalence
- Regular screening for high-risk groups, especially in immunocompromised individuals


