What are Encephaloceles?
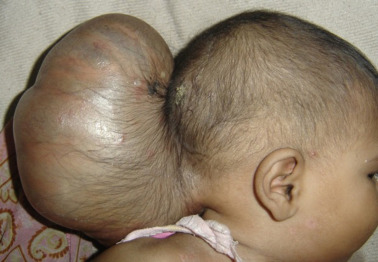
Encephaloceles, also known as brain herniation, are rare neural tube defects where brain tissue and the protective layers of the brain protrude through an abnormal opening in the skull. This condition occurs during fetal development, when the neural tube, which eventually forms the brain and spinal cord, fails to close properly. As a result, part of the brain or spinal cord may herniate through the skull, forming a sac-like structure that contains brain tissue or cerebrospinal fluid (CSF).
What Causes Encephaloceles?
The exact cause of encephaloceles is not always clear, but a combination of genetic and environmental factors can contribute to this condition. Some potential causes include:
1. Genetic Factors
In many cases, encephaloceles are linked to genetic abnormalities. If a parent has a history of neural tube defects or encephaloceles, there is an increased likelihood that the child may also be born with this condition. Some genetic syndromes, such as Meckel syndrome or Walker-Warburg syndrome, are associated with a higher risk of encephaloceles.
2. Nutritional Deficiencies
Lack of folic acid during pregnancy is a well-known risk factor for neural tube defects, including encephaloceles. Folic acid is a crucial nutrient that helps the neural tube close properly during fetal development. Insufficient intake of folic acid before and during early pregnancy can significantly increase the risk of encephaloceles.
3. Environmental Factors
Exposure to certain environmental toxins or infections during pregnancy may contribute to the development of encephaloceles. For instance, maternal exposure to radiation or certain chemicals may increase the risk of this condition.
4. Pre-existing Maternal Health Conditions
Certain maternal health conditions, such as obesity, diabetes, or poorly controlled metabolic disorders, may increase the likelihood of having a baby with encephaloceles. Additionally, advanced maternal age may be a contributing factor.
What Are the Types of Encephaloceles?
Encephaloceles are classified based on their location and the type of brain tissue involved. The main types of encephaloceles include:
1. Occipital Encephalocele
This is the most common type of encephalocele and occurs at the back of the skull, in the area called the occipital bone. Brain tissue or cerebrospinal fluid may protrude from the opening. Children born with occipital encephaloceles typically experience neurological impairments such as developmental delays, motor dysfunction, and intellectual disabilities.
2. Frontal Encephalocele
This type occurs at the front of the skull, in the frontal bone. It may involve less brain tissue and is often smaller than occipital encephaloceles. However, it can still lead to issues such as facial deformities, vision problems, or developmental delays.
3. Basal Encephalocele
Basal encephaloceles occur at the base of the skull, where the skull meets the spine. These are much less common and are often associated with significant neurological complications due to the proximity to the brainstem and spinal cord.
4. Multiple or Complex Encephaloceles
In rare cases, a child may have more than one encephalocele or multiple brain herniations. These cases are typically associated with severe neurological impairment and may require more complex surgical intervention.
What Are the Symptoms of Encephaloceles?
The symptoms of encephaloceles can vary depending on the size and location of the brain herniation, as well as the amount of brain tissue involved. Some common symptoms include:
- Visible bulge or sac-like structure on the head, especially at the back or front of the skull
- Neurological issues, such as developmental delays or intellectual disabilities
- Motor impairments, including difficulty with movement or coordination
- Seizures
- Vision problems, including blindness or partial sight loss
- Hydrocephalus (accumulation of cerebrospinal fluid in the brain)
- Craniofacial deformities, such as cleft palate or facial asymmetry
- Learning difficulties and cognitive impairments
The severity of these symptoms can range from mild to severe, depending on the extent of the encephalocele and its associated complications.
How is Encephaloceles Diagnosed?
Encephaloceles are typically diagnosed before birth or shortly after delivery through imaging studies and physical examination. Some common diagnostic methods include:
1. Ultrasound
During pregnancy, an ultrasound can detect abnormalities in fetal development, including the presence of a bulging sac-like structure on the head. This is often the first step in diagnosing encephaloceles during pregnancy.
2. MRI (Magnetic Resonance Imaging)
After birth, an MRI is commonly used to obtain detailed images of the brain and skull. This can help determine the size and location of the encephalocele, as well as assess any associated brain tissue involvement or damage.
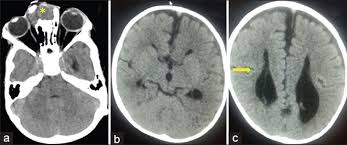
3. CT Scan
A CT scan may be used to get a clearer picture of the encephalocele and any related bone deformities. It is also helpful in planning surgical treatment.
4. Genetic Testing
If there is suspicion that the encephalocele is part of a genetic syndrome, genetic testing may be recommended. This can help identify underlying genetic conditions and inform management and treatment decisions.
How is Encephaloceles Treated?
The treatment of encephaloceles generally involves surgery to remove the herniated brain tissue and close the opening in the skull. The goals of treatment are to prevent further brain damage, reduce the risk of infection, and improve the child’s neurological function. Some common treatment approaches include:
1. Surgical Repair
Surgery is typically performed shortly after birth, especially if the encephalocele is large or causing significant neurological issues. During the surgery, the protruding brain tissue or CSF is carefully repositioned, and the skull opening is closed. The timing and approach to surgery depend on the size and location of the encephalocele, as well as the child’s overall health.
2. Hydrocephalus Management
If the child has hydrocephalus, they may require a shunt to help drain excess cerebrospinal fluid and relieve pressure on the brain. This is often an ongoing treatment that may require follow-up surgeries as the child grows.
3. Neurological Rehabilitation
Children who experience neurological impairments due to encephaloceles may benefit from physical therapy, speech therapy, and occupational therapy. These therapies help children develop motor skills, communication abilities, and cognitive functions.
4. Genetic Counseling
If the encephalocele is associated with a genetic syndrome, genetic counseling may be recommended for the family to understand the condition, its inheritance patterns, and potential risks for future pregnancies.
What is the Prognosis for Children with Encephaloceles?
The prognosis for children with encephaloceles depends on several factors, including the size and location of the encephalocele, the amount of brain tissue involved, and the presence of any associated medical conditions. Some children may experience only mild symptoms and grow up to lead relatively normal lives, while others may have significant neurological impairments that require lifelong support.
Children with smaller encephaloceles who undergo early surgical repair tend to have a better prognosis. However, larger encephaloceles or those involving the brainstem can lead to severe developmental and neurological challenges.


