What are Acral Ulcerations?
Acral ulcerations refer to open sores or wounds that develop on the extremities (hands, feet, fingers, and toes). These ulcers may result from poor circulation, infections, autoimmune diseases, or trauma. If left untreated, acral ulcers can lead to serious complications, including infection, tissue damage, or even amputation.
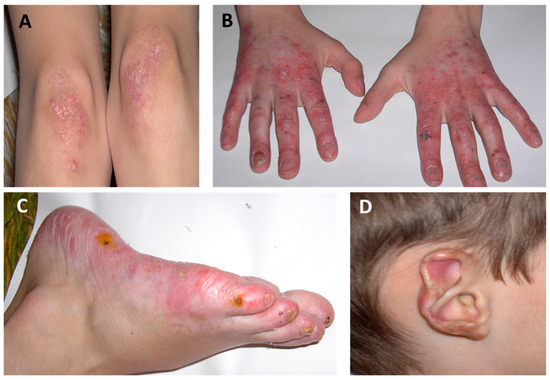
What Causes Acral Ulcerations?
Acral ulcers develop due to various underlying conditions that impair skin integrity, blood flow, or healing.
Common Causes:
- Peripheral artery disease (PAD) – Reduced blood flow to the extremities
- Diabetes (Diabetic foot ulcers) – Poor circulation and nerve damage
- Autoimmune disorders (e.g., lupus, scleroderma, vasculitis) – Inflammatory damage to blood vessels
- Infections (Bacterial, fungal, or viral) – Compromised skin leading to sores
- Frostbite or burns – Skin tissue damage leading to ulcer formation
- Pressure ulcers (bedsores) – Prolonged pressure restricting blood flow
- Neuropathy – Loss of sensation increases the risk of unnoticed injuries
- Malignancy (Cancerous ulcers) – Skin cancer leading to non-healing wounds
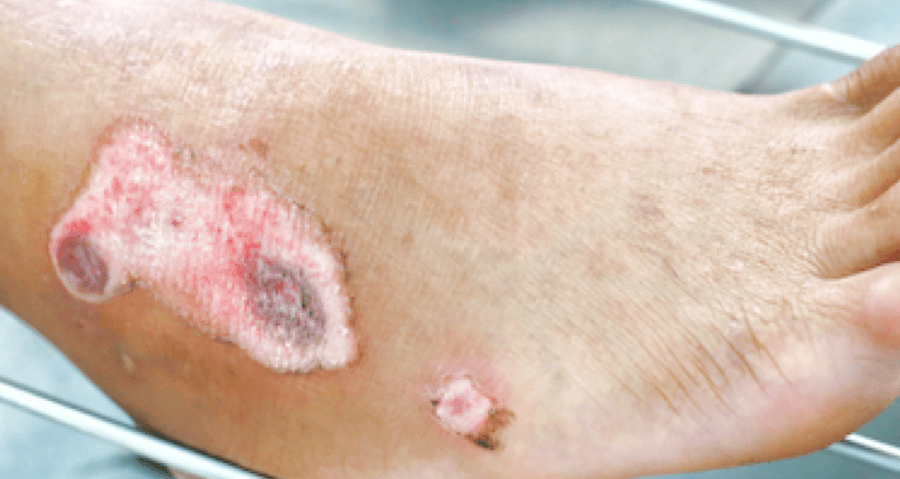
What Are the Symptoms of Acral Ulcerations?
Acral ulcers may vary in severity, from small, superficial wounds to deep, non-healing sores.
Common Signs & Symptoms:
- Open sores or wounds on fingers, toes, hands, or feet
- Pain, tenderness, or numbness around the affected area
- Swelling, redness, or warmth (possible infection)
- Discolored or blackened skin (tissue necrosis)
- Pus, drainage, or foul odor (signs of infection)
- Delayed wound healing or recurrence
How Are Acral Ulcerations Diagnosed?
A medical evaluation is necessary to determine the underlying cause and treatment approach.
Diagnostic Tests:
- Physical Examination – Doctor assesses ulcer size, depth, and signs of infection
- Blood Tests – Checks for diabetes, infections, or autoimmune diseases
- Doppler Ultrasound – Evaluates blood flow to extremities
- Skin Biopsy – Identifies underlying skin conditions or malignancies
- Wound Culture – Detects bacterial or fungal infections
What Are the Treatment Options for Acral Ulcerations?
Treatment focuses on healing the ulcer, managing underlying conditions, and preventing complications.
1. Wound Care & Management
- Cleaning the ulcer with saline – Prevents infection
- Dressing changes – Uses moist dressings, hydrocolloids, or antimicrobial bandages
- Debridement (removal of dead tissue) – Promotes healing
2. Medications & Therapies
- Antibiotics – If bacterial infection is present
- Pain management (NSAIDs or analgesics) – Reduces discomfort
- Topical wound healing agents – Growth factors or skin substitutes for chronic ulcers
3. Addressing Underlying Conditions
- Diabetes control – Blood sugar management to prevent ulcers
- Improving circulation – Lifestyle changes, medications, or vascular surgery
- Autoimmune treatment – Corticosteroids or immunosuppressants if related to autoimmune disease
4. Advanced Treatments for Chronic Ulcers
- Hyperbaric oxygen therapy (HBOT) – Increases oxygen supply to aid healing
- Skin grafting – For severe, non-healing ulcers
- Amputation (In extreme cases) – If tissue death spreads
Can Acral Ulcerations Cause Complications?
If left untreated, acral ulcers can lead to:
- Infections (cellulitis, osteomyelitis, gangrene)
- Permanent tissue damage
- Limb amputation in severe cases


