what is Amyotrophic Lateral Sclerosis (ALS)?
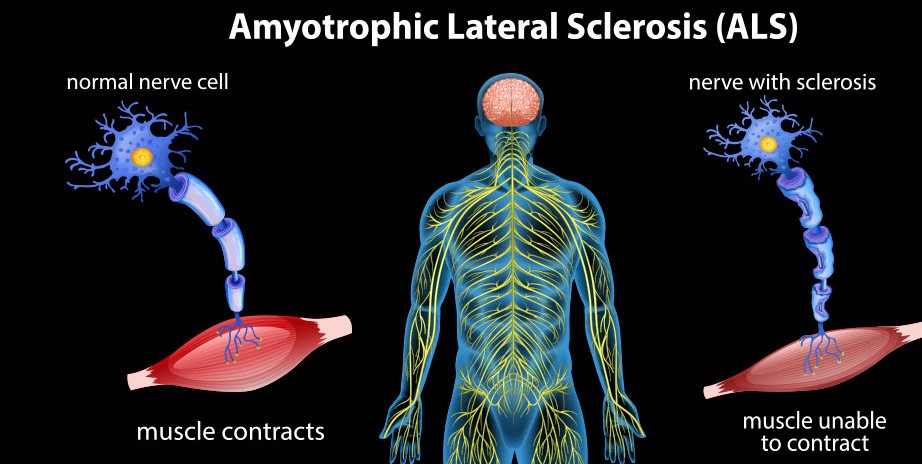
Amyotrophic Lateral Sclerosis (ALS), also known as Lou Gehrig’s disease, is a progressive neurological disorder that affects nerve cells in the brain and spinal cord. ALS leads to the gradual loss of voluntary muscle movement, eventually causing paralysis. Over time, the condition impacts essential functions like speaking, swallowing, and breathing.
While ALS does not affect cognitive function in most cases, some individuals may experience mild changes in thinking or behavior. Currently, there is no cure for ALS, but treatment can help manage symptoms and improve quality of life.
What Are the Symptoms of ALS?
ALS symptoms vary from person to person and worsen over time. Early signs are often subtle and may go unnoticed. Common symptoms include:
Early Symptoms:
- Muscle weakness in the hands, legs, feet, or arms.
- Difficulty gripping objects or performing fine motor tasks.
- Muscle cramps and twitching (fasciculations), especially in the arms, legs, or tongue.
- Slurred speech or trouble swallowing.
- Unsteady walking and frequent falls.
Progressive Symptoms:
- Increasing muscle stiffness (spasticity) and loss of muscle control.
- Difficulty speaking (dysarthria) and swallowing (dysphagia).
- Weight loss due to muscle deterioration.
- Shortness of breath and breathing difficulties as respiratory muscles weaken.
- Emotional changes such as excessive laughing or crying (pseudobulbar affect).
Advanced Symptoms:
- Complete loss of voluntary muscle movement.
- Paralysis, requiring a feeding tube and ventilatory support.
- Inability to speak, leading to communication through assistive devices.
- Severe respiratory failure, which is the leading cause of death in ALS patients.
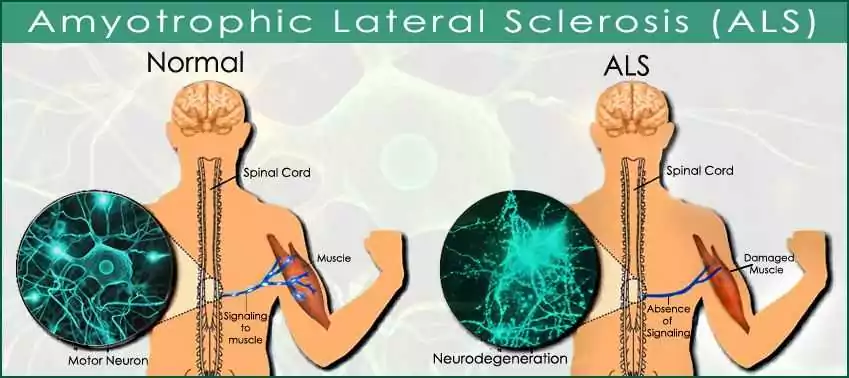
What Causes ALS?
The exact cause of ALS is unknown, but researchers believe it results from a combination of genetic and environmental factors.
Genetic Factors (Familial ALS – 5-10% of Cases)
- Mutations in Genes – Mutations in the C9orf72, SOD1, TARDBP, and FUS genes have been linked to ALS.
- Family History – If ALS runs in the family, there is a higher risk of inheriting the disease.
Environmental Factors (Sporadic ALS – 90-95% of Cases)
- Exposure to Toxins – Exposure to chemicals like pesticides, heavy metals, or lead may increase risk.
- Physical Trauma – Head injuries and repeated concussions have been associated with ALS.
- Military Service – Higher rates of ALS have been reported among veterans, possibly due to environmental exposures.
- Viral Infections – Some studies suggest viruses may contribute to motor neuron damage.
Biological Mechanisms Involved in ALS:
- Glutamate Toxicity – Excess glutamate, a neurotransmitter, can damage nerve cells.
- Oxidative Stress – Free radicals can harm motor neurons.
- Mitochondrial Dysfunction – Energy production failure leads to cell death.
- Abnormal Protein Aggregation – Toxic protein clumps accumulate in motor neurons.
How Is ALS Diagnosed?
ALS is difficult to diagnose in its early stages because its symptoms resemble other neurological conditions. A comprehensive evaluation includes:
Medical History and Physical Examination:
- Assessment of muscle weakness, reflexes, and coordination.
- Review of family history and environmental exposures.
Diagnostic Tests:
- Electromyography (EMG) – Measures electrical activity in muscles to detect nerve dysfunction.
- Nerve Conduction Studies (NCS) – Assesses how well nerves transmit signals.
- MRI (Magnetic Resonance Imaging) – Helps rule out other conditions like multiple sclerosis or tumors.
- Spinal Tap (Lumbar Puncture) – Analyzes cerebrospinal fluid for abnormalities.
- Genetic Testing – Determines if familial ALS is present.
- Blood and Urine Tests – Checks for metabolic disorders or infections that mimic ALS.
A definitive ALS diagnosis is made when progressive motor neuron degeneration is confirmed without signs of another neurological disorder.
How Is ALS Treated?
While there is no cure, treatments focus on slowing disease progression, relieving symptoms, and improving quality of life.
Medications:
- Riluzole (Rilutek) – Slows ALS progression by reducing glutamate levels.
- Edaravone (Radicava) – Helps slow functional decline in some patients.
- Muscle Relaxants (e.g., Baclofen, Tizanidine) – Reduces muscle spasticity and stiffness.
- Antidepressants and Anti-Anxiety Medications – Manages emotional distress.
- Pseudobulbar Affect Medications (e.g., Nuedexta) – Controls uncontrollable laughing or crying episodes.
Physical and Occupational Therapy:
- Helps maintain mobility and improve muscle function.
- Uses assistive devices (wheelchairs, braces, walkers) for movement support.
Speech and Swallowing Therapy:
- Helps patients communicate using voice amplifiers, speech-generating devices, or eye-tracking technology.
- Provides techniques for safer swallowing and reducing choking risk.
Respiratory Support:
- Non-invasive ventilation (BiPAP) can help ease breathing difficulties.
- A tracheostomy may be necessary in advanced stages for mechanical ventilation.
Nutritional Support:
- High-calorie diets help prevent malnutrition due to difficulty swallowing.
- Feeding tubes (PEG tubes) may be required in later stages.
Experimental Treatments and Clinical Trials:
- Gene therapy, stem cell therapy, and new medications are being studied for ALS treatment.
How Does ALS Affect the Body and Mind?
Physical Impact:
- Progressive loss of muscle control and strength.
- Increased difficulty performing everyday activities.
- Dependence on caregivers for mobility, feeding, and communication.
Cognitive and Emotional Effects:
- Some patients develop Frontotemporal Dementia (FTD), causing memory and behavior changes.
- High risk of depression and anxiety due to disease progression.
Social and Financial Burden:
- Patients require long-term care, assistive technology, and home modifications.
- Emotional strain on family members and caregivers.
What Are the Long-Term Effects of ALS?
ALS leads to total muscle paralysis and, ultimately, respiratory failure. Without ventilation support, the life expectancy after diagnosis is 2 to 5 years, though some individuals (e.g., Stephen Hawking) have lived much longer.
Long-term effects include:
- Complete loss of mobility and independence.
- Inability to speak, swallow, or breathe without assistance.
- Increased risk of infections (e.g., pneumonia).
How to Manage ALS for a Better Quality of Life
For Individuals Living with ALS:
- Engage in physical therapy to maintain mobility for as long as possible.
- Use adaptive equipment for communication and daily activities.
- Consider joining an ALS support group for emotional and psychological support.
For Caregivers & Families:
- Provide a comfortable and supportive home environment.
- Learn about assistive devices and care techniques.
- Seek respite care or professional help when needed.
For Communities & Healthcare Providers:
- Increase ALS awareness and advocacy for better treatments.
- Improve accessibility for individuals with physical disabilities.
- Support ongoing research and fundraising efforts for a cure.


