intraduction
Autoimmune Retinopathy is a rare condition where the body’s immune system attacks the retina, leading to vision problems and potential blindness. This disorder can occur as a result of an autoimmune response to the retina or associated tissues, affecting individuals in different ways. In this article, we will explore the symptoms, causes, diagnosis, and treatment options for Autoimmune Retinopathy.
What is Autoimmune Retinopathy?
Autoimmune Retinopathy refers to a condition where the body’s immune system mistakenly targets and attacks the retina, the light-sensitive tissue at the back of the eye. The retina plays a vital role in vision by converting light into nerve signals that are sent to the brain. When the immune system attacks the retina, it can cause inflammation, damage, and impair the ability to see clearly.
While Autoimmune Retinopathy is rare, it can be part of a larger autoimmune disorder or occur as a primary condition. It may cause symptoms that range from mild vision disturbances to severe vision loss. The condition can affect individuals of any age, but it is more commonly diagnosed in adults.
What Causes Autoimmune Retinopathy?
The exact cause of Autoimmune Retinopathy is not fully understood, but it is believed to result from the body’s immune system malfunctioning and attacking the retina as if it were a foreign invader. Several potential causes and risk factors include:
1. Autoimmune Disorders?
- Autoimmune Retinopathy is most commonly associated with other autoimmune diseases such as Systemic Lupus Erythematosus (SLE), Rheumatoid Arthritis, Thyroiditis, or Sarcoidosis. These conditions trigger an overactive immune response, leading the body to mistakenly attack its own tissues, including the retina.
2. Immune System Dysfunction?
- The immune system produces antibodies that target specific components of the retina, particularly the retinal antigen. This can result in inflammation and damage to the retinal cells, leading to a loss of vision.
3. Genetic Factors?
- Certain genetic factors may predispose individuals to develop autoimmune disorders that could lead to Autoimmune Retinopathy. However, more research is needed to identify specific genes involved.
4. Infections or Environmental Triggers?
- In some cases, infections or other environmental triggers may provoke the onset of autoimmune diseases or inflammation in the retina, though the connection remains largely unexplained.
What Are the Symptoms of Autoimmune Retinopathy?
The symptoms of Autoimmune Retinopathy can vary depending on the severity of the condition. Common symptoms include:
1. Vision Impairment?
- The most common symptom is blurry vision or difficulty seeing clearly. The vision may appear distorted or out of focus, especially in low-light conditions.
2. Night Blindness?
- Night blindness or difficulty seeing in dim light is another common symptom. This occurs due to damage to the retinal cells responsible for vision in low-light environments.
3. Flashes of Light or Floaters?
- Some individuals experience flashes of light or the appearance of floaters in their field of vision. These are caused by retinal changes or inflammation affecting the optic nerve.
4. Peripheral Vision Loss?
- Autoimmune Retinopathy can cause a loss of peripheral vision (side vision), leading to difficulty in seeing objects outside of a central focus.
5. Color Vision Abnormalities?
- Some individuals with Autoimmune Retinopathy may notice a loss of color vision or changes in how colors appear.
6. Progressive Vision Loss?
- If left untreated, Autoimmune Retinopathy can result in progressive vision loss and even complete blindness in severe cases.
How is Autoimmune Retinopathy Diagnosed?
The diagnosis of Autoimmune Retinopathy typically involves a combination of clinical examination, specialized eye tests, and blood work.
1. Ophthalmologic Examination?
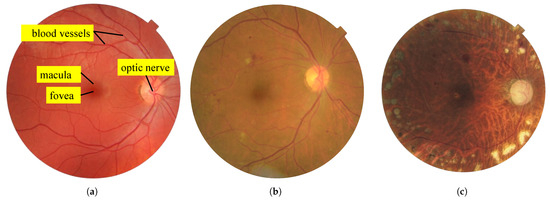
- A thorough eye exam performed by an ophthalmologist is essential for diagnosing Autoimmune Retinopathy. The doctor will check for signs of retinal inflammation, blood vessel abnormalities, and other damage to the retina.
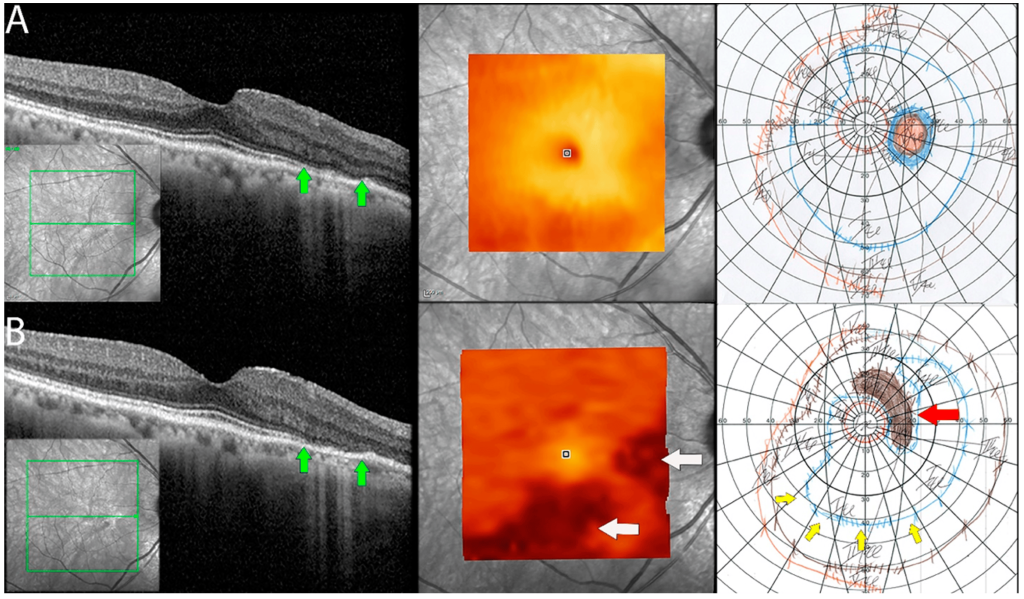
- Fundus Photography or Optical Coherence Tomography (OCT) can be used to capture detailed images of the retina, showing any abnormalities.
2. Electroretinography (ERG)?
- Electroretinography (ERG) measures the electrical responses of the retina to light stimuli. It can help determine the extent of retinal dysfunction and assess how well the retina is responding to light.
3. Blood Tests?
- Blood tests may be performed to detect markers of autoimmune disease, such as elevated antinuclear antibodies (ANA) or specific antibodies related to the condition causing the autoimmune response (e.g., anti-Ro/SSA antibodies in lupus).
4. Genetic Testing?
- In some cases, genetic testing may be performed to assess for genetic predispositions to autoimmune disorders that could contribute to retinal damage.
What Are the Treatment Options for Autoimmune Retinopathy?
The treatment of Autoimmune Retinopathy aims to control inflammation, slow disease progression, and preserve vision. Since it is an autoimmune condition, treatment often involves addressing the underlying immune system dysfunction.
1. Immunosuppressive Therapy?
- Corticosteroids such as prednisone are commonly prescribed to reduce inflammation and suppress the immune response attacking the retina. In some cases, other immunosuppressive drugs, such as azathioprine or methotrexate, may be used to control the autoimmune activity.
2. Plasmapheresis?
- Plasmapheresis, a procedure that filters out harmful antibodies from the blood, may be recommended in severe cases to reduce the presence of autoantibodies affecting the retina.
3. Biologic Therapies?
- Biologic therapies, such as rituximab, may be considered in cases where traditional immunosuppressive therapy is not effective.
4. Anti-Inflammatory Medications?
- Non-steroidal anti-inflammatory drugs (NSAIDs) may be used to control mild inflammation and reduce discomfort, although these are typically used in conjunction with stronger treatments.
5. Management of Underlying Autoimmune Disease?
- If Autoimmune Retinopathy is secondary to an underlying autoimmune disease (such as lupus or rheumatoid arthritis), treatment may involve managing the primary condition to control the immune system’s overactivity.
6. Vision Rehabilitation?
- In cases of significant vision loss, vision rehabilitation therapies may be recommended. This includes low vision aids, specialized glasses, or training to help the individual adapt to reduced vision.
7. Monitoring and Follow-Up?
- Ongoing monitoring of the retina and immune system is essential for managing the condition. Regular eye exams and blood tests are necessary to assess the progression of the disease and adjust treatment as needed.
What is the Prognosis for Autoimmune Retinopathy?
The prognosis for Autoimmune Retinopathy depends on the severity of the condition, how early it is diagnosed, and how well it responds to treatment. Early intervention can help slow the progression of the disease and preserve vision. However, if left untreated, Autoimmune Retinopathy can lead to irreversible damage and blindness.
1. With Proper Treatment?
- With appropriate treatment, including immunosuppressive therapy and management of underlying autoimmune conditions, individuals may be able to stabilize their vision and prevent further deterioration.
2. Without Treatment?
- If Autoimmune Retinopathy is not treated promptly, it can cause irreversible vision loss due to ongoing retinal damage. The degree of vision impairment can vary widely from person to person.
Can Autoimmune Retinopathy Be Prevented?
Currently, there is no known way to prevent Autoimmune Retinopathy. However, early detection and management of autoimmune diseases and retinal inflammation can help prevent or minimize the damage caused by this condition. Regular eye exams and blood tests are crucial for individuals with autoimmune diseases to catch any early signs of retinal involvement.


