intraduction
Autoimmune diseases are a group of disorders where the body’s immune system mistakenly attacks its own healthy tissues. Normally, the immune system protects the body from infections and foreign invaders, but in autoimmune diseases, this system goes awry. In this article, we will explore the causes, symptoms, diagnosis, and treatment options for autoimmune diseases.
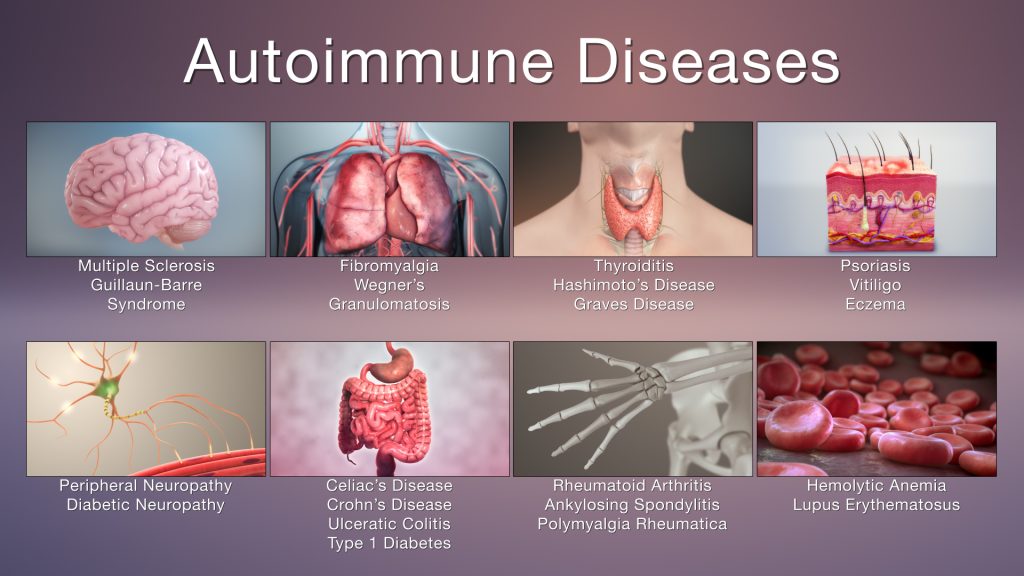
What are Autoimmune Diseases?
Autoimmune diseases occur when the body’s immune system becomes confused and starts attacking its own cells, tissues, or organs. This leads to inflammation, damage, and dysfunction in various parts of the body. There are over 80 known autoimmune diseases, which can affect a range of systems in the body, including the skin, joints, muscles, blood vessels, nerves, and organs.
Common Autoimmune Diseases:
- Rheumatoid Arthritis
- Systemic Lupus Erythematosus (SLE)
- Multiple Sclerosis (MS)
- Type 1 Diabetes
- Graves’ Disease
- Hashimoto’s Thyroiditis
- Celiac Disease
- Psoriasis
What Causes Autoimmune Diseases?
The exact cause of autoimmune diseases is not fully understood, but several factors may contribute to their development. Some of the common causes include:
1. Genetic Factors?
- Genetics play a significant role in the development of autoimmune diseases. People with a family history of autoimmune disorders are more likely to develop one themselves. Specific genes have been identified that may predispose individuals to autoimmune diseases.
2. Environmental Triggers?
- Certain environmental factors such as infections (viruses or bacteria), smoking, or exposure to chemicals can trigger or exacerbate autoimmune responses in individuals who are genetically predisposed.
3. Hormonal Factors?
- Autoimmune diseases are more common in women, suggesting that hormones such as estrogen may contribute to the development of these conditions.
4. Immune System Dysregulation?
- In autoimmune diseases, the immune system fails to distinguish between the body’s own healthy cells and foreign invaders. This results in the immune system attacking normal tissues, leading to inflammation and damage.
What are the Symptoms of Autoimmune Diseases?
The symptoms of autoimmune diseases vary widely depending on the specific condition and the organs or tissues affected. Common symptoms across many autoimmune diseases include:
1. Fatigue and Weakness?
- Persistent fatigue is one of the most common symptoms of autoimmune diseases. People with autoimmune conditions often experience unexplained tiredness and a lack of energy.
2. Joint Pain and Swelling?
- Many autoimmune diseases, such as rheumatoid arthritis, cause joint pain, swelling, and stiffness. These symptoms are usually worse in the morning or after periods of inactivity.
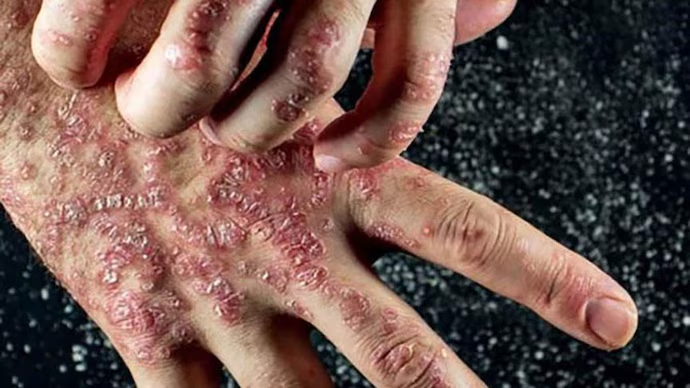
3. Skin Problems?
- Skin rashes, redness, and irritation are common in autoimmune diseases like lupus and psoriasis. Some individuals may experience dry skin or discoloration of the skin.
4. Digestive Issues?
- Conditions such as celiac disease and Crohn’s disease can cause digestive problems like diarrhea, abdominal pain, bloating, and malnutrition.
5. Hair Loss?
- Certain autoimmune diseases like lupus or alopecia areata can cause hair loss or thinning.
6. Fever and Swollen Lymph Nodes?
- Autoimmune diseases can lead to systemic inflammation, causing fever and swollen lymph nodes.
7. Neurological Symptoms?
- Some autoimmune conditions like multiple sclerosis can affect the nervous system, leading to symptoms such as numbness, tingling, dizziness, and difficulty walking.
How Are Autoimmune Diseases Diagnosed?
Diagnosing autoimmune diseases can be challenging due to the variety of symptoms and the overlap with other conditions. However, a combination of the following methods can help establish a diagnosis:
1. Medical History and Physical Examination?
- A doctor will typically start with a thorough medical history and physical examination, looking for signs and symptoms of autoimmune disease.
2. Blood Tests?
- Antibody tests, such as antinuclear antibody (ANA) tests, are often used to detect abnormal immune system activity.
- Specific tests, like the rheumatoid factor (RF) or anti-CCP antibodies, may help diagnose diseases like rheumatoid arthritis.
- Other markers, such as C-reactive protein (CRP) or erythrocyte sedimentation rate (ESR), may be elevated in autoimmune diseases due to inflammation.
3. Imaging and Biopsy?
- Imaging studies like X-rays, MRIs, or CT scans may be used to assess organ damage or inflammation caused by autoimmune diseases.
- Tissue biopsy may be performed if organ involvement is suspected.
4. Genetic Testing?
- Genetic testing can help identify specific markers or genes associated with autoimmune diseases, although it is not a definitive diagnostic tool on its own.
What Are the Treatment Options for Autoimmune Diseases?
There is no universal cure for autoimmune diseases, but there are several treatment options to manage symptoms, reduce inflammation, and prevent further damage to the body. Treatment typically involves a combination of medications, lifestyle changes, and sometimes, physical therapy. Common treatment options include:
1. Immunosuppressive Medications?
- Corticosteroids (e.g., prednisone) are often used to reduce inflammation and suppress the immune system’s attack on the body.
- Disease-modifying antirheumatic drugs (DMARDs), such as methotrexate, are used to slow the progression of diseases like rheumatoid arthritis.
- Biologic therapies target specific parts of the immune system to reduce inflammation and symptoms, such as TNF inhibitors for rheumatoid arthritis or interleukin inhibitors for other diseases.
2. Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)?
- NSAIDs, like ibuprofen, are commonly used to relieve pain, reduce swelling, and alleviate fever associated with autoimmune diseases.
3. Physical and Occupational Therapy?
- Physical therapy can help individuals maintain mobility and strength. Occupational therapy focuses on helping patients maintain independence in daily activities.
4. Dietary Changes and Supplements?
- For autoimmune diseases like celiac disease, following a gluten-free diet is essential. People with autoimmune diseases may also benefit from anti-inflammatory diets that include omega-3 fatty acids, antioxidants, and fiber.
- Supplements such as vitamin D, calcium, and probiotics may help improve overall health and reduce the effects of certain autoimmune conditions.
5. Plasma Exchange or Intravenous Immunoglobulin (IVIG)?
- For some severe autoimmune diseases, plasma exchange (plasmapheresis) or IVIG may be used to remove harmful antibodies or boost the immune system’s ability to fight inflammation.
Can Autoimmune Diseases Be Prevented?
Currently, there is no known way to prevent autoimmune diseases, as they are largely influenced by genetic and environmental factors. However, certain lifestyle changes can help reduce the risk of autoimmune diseases or manage the symptoms:
1. Healthy Diet?
- Eating a balanced, nutrient-rich diet can help support immune function and reduce inflammation.
2. Regular Exercise?
- Regular physical activity can help maintain joint function, improve cardiovascular health, and boost the immune system.
3. Avoid Smoking and Toxins?
- Smoking and exposure to certain environmental toxins can increase the risk of developing autoimmune diseases or trigger flare-ups.
4. Manage Stress?
- Chronic stress can trigger autoimmune disease flares. Practices like yoga, meditation, and mindfulness can help manage stress levels.
What is the Prognosis for Autoimmune Diseases?
The prognosis for autoimmune diseases varies depending on the specific condition, how early it is diagnosed, and how effectively it is treated. Some autoimmune diseases can be controlled with medication and lifestyle changes, allowing individuals to lead relatively normal lives. However, others may cause long-term complications or organ damage.
Early detection, prompt treatment, and ongoing care are essential for improving the prognosis of autoimmune diseases and preventing severe complications.


