What is Lower Limb Ischemia?
Lower limb ischemia refers to a condition where there is a reduced blood flow to the legs, leading to insufficient oxygen and nutrients being supplied to the muscles and tissues of the lower limbs. This condition can result from various causes, including narrowing or blockage of the arteries, leading to pain, tissue damage, and, in severe cases, limb loss.
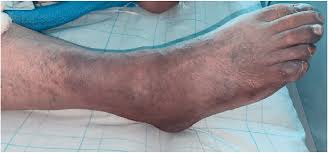
Types of Lower Limb Ischemia?
There are two main types of lower limb ischemia:
- Acute Lower Limb Ischemia?
- This occurs suddenly and is typically the result of an embolism (a clot or other material blocking an artery) or thrombosis (formation of a clot within a blood vessel).
- It is a medical emergency, as it can rapidly lead to tissue death and require urgent intervention.
- Chronic Lower Limb Ischemia?
- This develops gradually, typically due to atherosclerosis (plaque buildup) in the arteries over time, narrowing the blood vessels and restricting blood flow.
- Symptoms may progress slowly, causing discomfort and functional limitations but may not always be immediately life-threatening.
Causes of Lower Limb Ischemia?
Lower limb ischemia is caused by a variety of conditions that affect the blood vessels, including:
1. Atherosclerosis?
Atherosclerosis is the most common cause of chronic lower limb ischemia. It occurs when plaque (composed of fat, cholesterol, and other substances) builds up on the inner walls of the arteries, narrowing them and restricting blood flow. Over time, this can lead to severe ischemia.
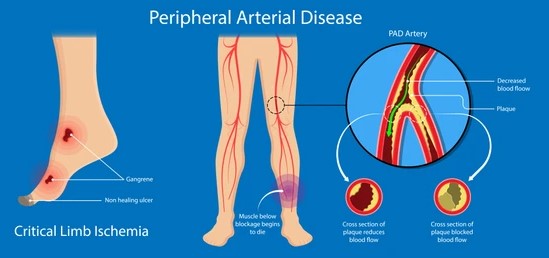
2. Peripheral Artery Disease (PAD)?
Peripheral artery disease is a type of atherosclerosis that affects the arteries supplying blood to the legs. It is a key cause of chronic lower limb ischemia, leading to symptoms like leg pain (especially during walking), numbness, and cramping.
3. Embolism?
An embolism occurs when a clot or other substance (such as fat or air) travels through the bloodstream and becomes lodged in a smaller artery in the leg, blocking blood flow. This can cause acute ischemia and needs immediate attention to restore circulation.
4. Thrombosis?
Thrombosis refers to the formation of a blood clot within an artery or vein. When a blood clot forms in an artery supplying the lower limb, it can reduce or completely block blood flow, leading to ischemia. It can be caused by factors such as diabetes, high blood pressure, and smoking.
5. Vasculitis?
Vasculitis is inflammation of the blood vessels, which can lead to damage to the arterial walls, reducing blood flow to the lower limbs. This is more common in certain autoimmune diseases such as Buerger’s disease or Takayasu’s arteritis.
6. Diabetes and High Blood Sugar?
Diabetes can contribute to vascular damage over time, leading to the development of lower limb ischemia. High blood sugar levels damage the blood vessels, making them more prone to atherosclerosis and blood clots.
7. Trauma or Injury?
In some cases, a trauma to the leg can cause damage to the blood vessels, resulting in impaired circulation and ischemia. Fractures, dislocations, or severe contusions can disrupt blood flow.
8. Smoking?
Smoking is a major risk factor for lower limb ischemia as it accelerates the process of atherosclerosis and damages blood vessels, reducing blood flow to the legs. Smokers are more likely to develop peripheral artery disease and experience lower limb ischemia.
9. High Blood Pressure?
Chronic high blood pressure (hypertension) can damage blood vessels over time, making them more susceptible to blockages and narrowing, which can lead to ischemia.
10. Hyperlipidemia (High Cholesterol)?
Elevated cholesterol levels can lead to the buildup of plaque in the arteries, contributing to the development of atherosclerosis and lower limb ischemia.
Symptoms of Lower Limb Ischemia?
The symptoms of lower limb ischemia can vary depending on the severity of the condition and whether the ischemia is acute or chronic:
Acute Symptoms (Acute Lower Limb Ischemia):
- Sudden and severe pain in the affected leg
- Pale, cool skin on the leg or foot
- Loss of pulses in the affected limb
- Numbness or paralysis in the leg
- Loss of sensation or function in the leg
- Severe swelling or gangrene (if left untreated)
Acute lower limb ischemia is a medical emergency and requires immediate attention to restore blood flow and prevent permanent damage.
Chronic Symptoms (Chronic Lower Limb Ischemia):
- Intermittent claudication: Pain, cramping, or tiredness in the leg muscles that occurs with walking or exercise and goes away with rest.
- Coldness or coolness in the legs or feet
- Leg numbness or weakness
- Shiny skin or hair loss on the legs
- Wounds or ulcers on the legs that do not heal
- Reduced toenail growth or changes in skin color
As chronic ischemia progresses, these symptoms can worsen, and individuals may experience rest pain, which is pain that occurs even at rest, especially at night.
Diagnosis of Lower Limb Ischemia?
The diagnosis of lower limb ischemia involves a thorough medical evaluation, including the following:
1. Physical Examination
A healthcare provider will begin with a physical exam, checking for visible signs of poor circulation, such as pale skin, cool extremities, and weak pulses in the legs or feet. They may also test for intermittent claudication and assess any wounds or ulcers.
2. Ankle-Brachial Index (ABI)
The Ankle-Brachial Index (ABI) is a simple and non-invasive test that compares the blood pressure in the ankles to the blood pressure in the arms. A low ABI indicates poor blood flow to the lower limbs and may suggest peripheral artery disease (PAD).
3. Ultrasound
Doppler ultrasound can be used to assess blood flow in the arteries of the legs. This imaging test helps identify areas of blockage or narrowing in the arteries.
4. CT Angiography or MR Angiography
These imaging techniques are used to get detailed pictures of the arteries in the legs and identify any blockages, narrowing, or aneurysms. They may be used to plan further treatment, such as surgery or endovascular procedures.
5. Arteriography
In some cases, a more invasive procedure called angiography may be performed. This involves injecting a contrast dye into the arteries and taking X-ray images to visualize the blood vessels and detect any blockages or abnormalities.
Treatment of Lower Limb Ischemia?
The treatment of lower limb ischemia depends on the cause, severity, and type of ischemia (acute or chronic):
1. Lifestyle Modifications?
- Smoking cessation is crucial for improving circulation and preventing further damage to blood vessels.
- Exercise (such as walking) is recommended to help improve circulation and reduce symptoms of intermittent claudication.
- Dietary changes to lower cholesterol and blood pressure can also help manage the condition.
2. Medications?
- Antiplatelet medications (e.g., aspirin or clopidogrel) to prevent blood clots.
- Statins to lower cholesterol levels and slow the progression of atherosclerosis.
- Blood pressure medications to control hypertension.
- Vasodilators to help open up blood vessels and improve blood flow.
3. Endovascular Procedures?
- Angioplasty and stent placement: A balloon is inflated in a narrowed artery to open it up, and a stent may be placed to keep it open.
- Thrombectomy: Removal of a blood clot causing an embolism or thrombosis to restore blood flow.
4. Surgical Treatment?
In some cases, surgery may be required to bypass a blocked artery or remove a blockage, such as:
- Bypass surgery: A graft is used to bypass a blocked artery and restore blood flow.
- Endarterectomy: Removal of plaque from the artery to improve blood flow.
5. Amputation?
In severe cases where the tissue is irreversibly damaged due to gangrene or necrosis, amputation of the affected limb may be necessary to prevent the spread of infection and protect the individual’s life.
Prevention of Lower Limb Ischemia?
To prevent lower limb ischemia or manage it effectively, the following steps are recommended:
- Control risk factors such as high blood pressure, diabetes, and high cholesterol.
- Avoid smoking and limit alcohol consumption.
- Exercise regularly to improve circulation and maintain a healthy weight.
- Monitor and manage blood sugar if diabetic.
- Get regular check-ups to screen for peripheral artery disease, especially if you have risk factors like smoking or a


