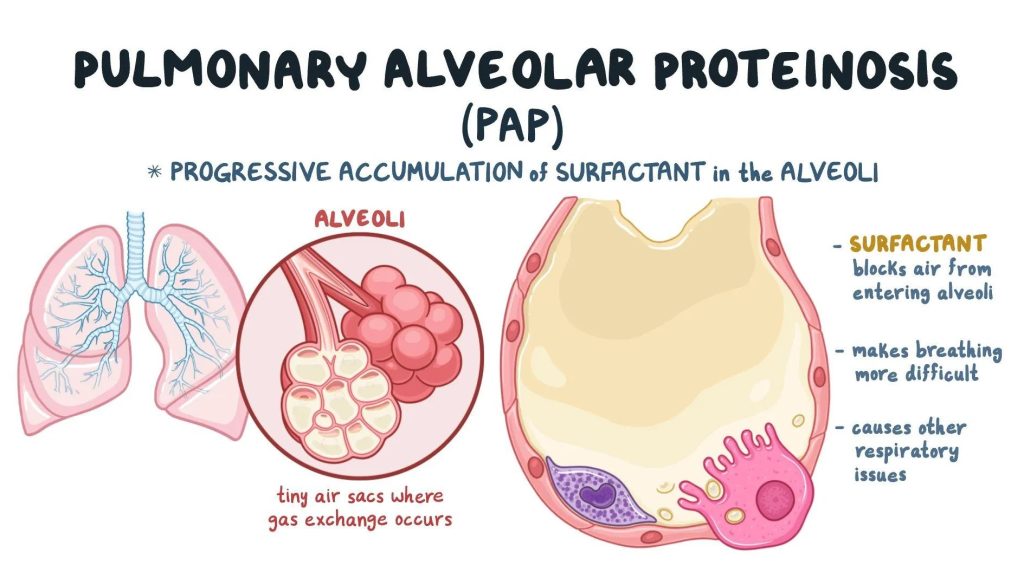
What is Alveolar Proteinosis?
Alveolar Proteinosis (AP) is a rare lung disease characterized by the buildup of surfactant (a fatty, protein-rich substance) in the air sacs (alveoli) of the lungs. This accumulation prevents proper oxygen exchange, leading to breathing difficulties and other complications. The condition can occur in different forms, including autoimmune, congenital, and secondary alveolar proteinosis.
What Are the Symptoms of Alveolar Proteinosis?
Symptoms of alveolar proteinosis can vary from mild to severe and may develop gradually over time. Common symptoms include:
- Shortness of breath (dyspnea)? – Especially noticeable during physical activity.
- Chronic cough? – Usually dry but can sometimes produce thick sputum.
- Fatigue and weakness? – Due to reduced oxygen levels in the blood.
- Chest discomfort? – A feeling of tightness or pressure in the chest.
- Cyanosis (bluish skin color)? – A sign of low oxygen levels.
- Frequent lung infections? – Increased risk of bacterial or fungal infections.
What Causes Alveolar Proteinosis?
The causes of alveolar proteinosis depend on its type:
1. Autoimmune Alveolar Proteinosis (PAP)?
- The most common form, caused by the immune system producing GM-CSF (granulocyte-macrophage colony-stimulating factor) autoantibodies, which prevent lung cells from clearing excess surfactant.
2. Congenital Alveolar Proteinosis?
- A rare, inherited condition caused by genetic mutations affecting surfactant production or clearance.
- Usually diagnosed in newborns or infants.
3. Secondary Alveolar Proteinosis?
- Develops as a result of other medical conditions, such as:
- Lung infections (tuberculosis, fungal infections).
- Toxic inhalation exposure (silica, dust, chemicals, or fumes).
- Blood disorders (leukemia, lymphoma).
- Immune system disorders (HIV, bone marrow diseases).
How is Alveolar Proteinosis Diagnosed?
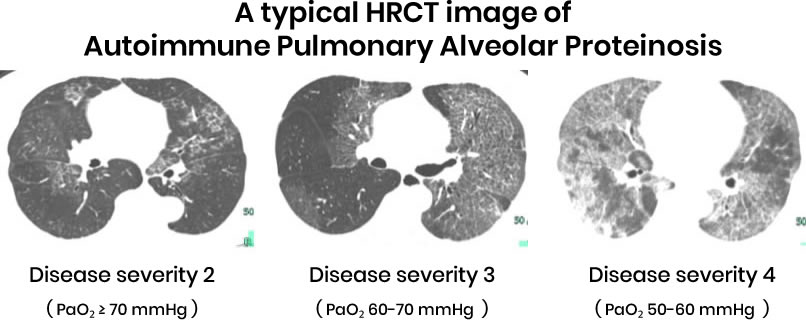
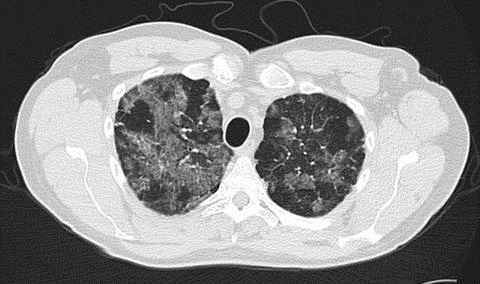
1. Chest X-ray or CT Scan?
- Shows “crazy paving” pattern, indicating lung abnormalities.
2. Pulmonary Function Tests (PFTs)?
- Measures lung capacity and oxygen exchange efficiency.
3. Bronchoalveolar Lavage (BAL)?
- Fluid is washed into and retrieved from the lungs to analyze surfactant buildup.
4. Blood Tests?
- Checks for GM-CSF autoantibodies, which confirm autoimmune PAP.
5. Lung Biopsy?
- A small lung tissue sample is taken for microscopic examination, usually done if other tests are inconclusive.
What Are the Treatment Options for Alveolar Proteinosis?
Treatment depends on the severity and type of alveolar proteinosis. Options include:
1. Whole Lung Lavage (WLL)
- A procedure where saline is flushed into the lungs to remove excess surfactant.
- Often necessary for autoimmune PAP and can significantly improve symptoms.
2. GM-CSF Therapy
- Used in autoimmune alveolar proteinosis to stimulate surfactant clearance.
- Can be administered as an injection or inhaled treatment.
3. Oxygen Therapy
- Helps improve oxygen levels in severe cases, especially in those experiencing respiratory distress.
4. Lung Transplantation
- In severe or congenital cases, lung transplant may be considered if other treatments are ineffective.
What is the Prognosis for Alveolar Proteinosis?
- Many patients respond well to whole lung lavage and GM-CSF therapy, leading to long-term symptom relief.
- Without treatment, severe cases may lead to respiratory failure.
- Regular monitoring and early intervention can help manage symptoms effectively.
Can Alveolar Proteinosis Be Prevented?
- Autoimmune and congenital forms cannot be prevented, but early diagnosis can improve outcomes.
- Secondary alveolar proteinosis may be prevented by avoiding exposure to toxic substances and managing underlying health conditions.


