What is Knee Arthritis?
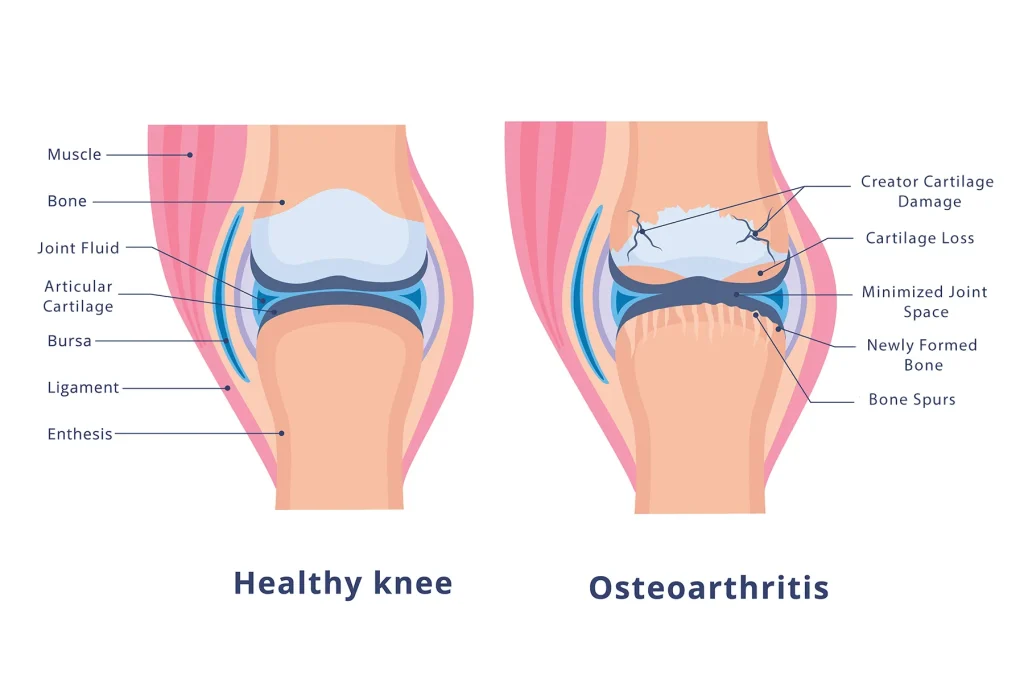
Knee arthritis is a condition where the cartilage in the knee joint gradually wears away, leading to pain, stiffness, swelling, and reduced mobility. It can affect one or both knees and is more common in older adults, though younger people can develop it due to injury or genetic factors.
There are several types of arthritis that can affect the knee, with osteoarthritis being the most common. Other types include rheumatoid arthritis, post-traumatic arthritis, and psoriatic arthritis.
What causes Knee Arthritis?
Knee arthritis can develop due to a variety of factors:
- Age-related wear and tear (osteoarthritis)
- Autoimmune disorders like rheumatoid or psoriatic arthritis
- Previous knee injuries such as fractures or ligament tears
- Repeated stress or overuse of the knee joint
- Obesity, which increases pressure on the knees
- Family history of arthritis
- Infections or metabolic conditions such as gout
These factors can lead to inflammation, breakdown of cartilage, and changes in the underlying bone.
What are the symptoms of Knee Arthritis?
Symptoms often develop gradually and may include:
- Persistent pain in or around the knee joint
- Swelling and warmth in the knee
- Stiffness, especially in the morning or after rest
- Grinding or popping sounds during movement
- Reduced range of motion
- Difficulty walking, climbing stairs, or standing for long periods
- Deformity in severe cases, such as bowing of the knee
Symptoms may worsen with activity and improve with rest.
How is Knee Arthritis diagnosed?
Diagnosis is based on a combination of:
- Medical history and symptom review
- Physical examination of the knee
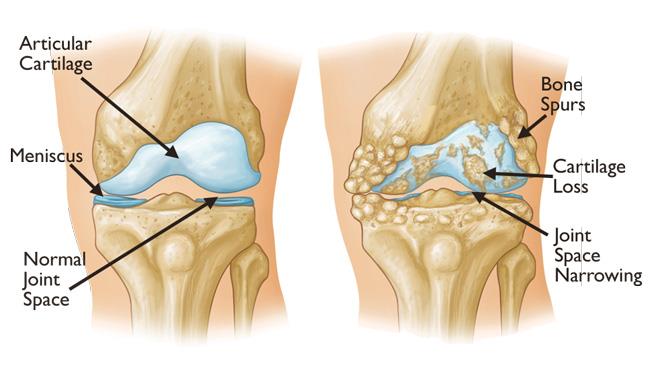
- X-rays to detect joint space narrowing, bone spurs, or changes in bone structure
- MRI scans to assess cartilage and soft tissue
- Blood tests to rule out autoimmune conditions
- Joint fluid analysis if infection or gout is suspected
Early diagnosis helps prevent progression and joint damage.
How is Knee Arthritis treated?
Treatment depends on the type and severity of arthritis. It may include:
Lifestyle and self-care:
- Weight loss to reduce knee stress
- Low-impact exercises like swimming or cycling
- Physical therapy to improve strength and flexibility
- Heat or cold therapy for pain relief
- Assistive devices like canes or knee braces
Medications:
- NSAIDs (e.g., ibuprofen, naproxen) for pain and inflammation
- Acetaminophen for mild pain
- Corticosteroid injections for flare-ups
- Hyaluronic acid injections to lubricate the joint
- DMARDs or biologics for autoimmune arthritis
Surgical options:
- Arthroscopy to remove loose cartilage or repair damage (less commonly used)
- Osteotomy to realign the knee joint
- Partial or total knee replacement in advanced cases
What is the recovery outlook?
The outlook depends on the type of arthritis and how early it is treated. With proper management:
- Mild cases can be controlled with lifestyle changes and medications
- Moderate cases may require injections or physical therapy
- Severe arthritis may eventually need joint replacement, which often leads to significant improvement in function and pain relief
Long-term commitment to joint care and follow-up is key to maintaining quality of life.
Can Knee Arthritis be prevented?
While not all cases can be prevented, the risk can be reduced by:
- Maintaining a healthy weight
- Exercising regularly to keep joints flexible
- Avoiding repetitive strain and high-impact sports
- Treating injuries promptly
- Managing chronic conditions like diabetes or autoimmune diseases


