A group of skin conditions involving thickening or overgrowth of the outer skin layer (keratin)
What is Keratosis?
Keratosis refers to a group of skin disorders characterized by the excessive growth or buildup of keratin, a protein that protects the skin. This results in rough, scaly, or hardened patches of skin. Keratosis is a broad term and includes several distinct types, some of which are harmless while others may carry a risk of progressing to skin cancer.
Keratosis can be benign (non-cancerous) or precancerous, and it is especially common in older adults or individuals with sun-damaged skin.
What causes Keratosis?
The causes depend on the type of keratosis, but common contributing factors include:
- Chronic sun exposure (especially for actinic keratosis)
- Aging
- Genetics (especially in inherited forms like keratosis pilaris)
- Skin damage or inflammation
- Viral infections (in some cases, such as in seborrheic keratosis)
- Impaired skin cell turnover
Who is at risk?
- Older adults, especially over age 40
- People with fair skin and history of sun exposure
- Individuals with a family history of keratosis
- Those with dry or sensitive skin
- People with weakened immune systems
What are the common types of Keratosis?
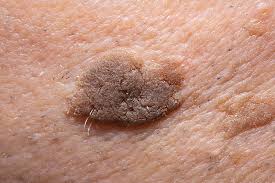
1. Actinic Keratosis (Solar Keratosis)
- Caused by sun damage
- Appears as rough, scaly patches on sun-exposed areas (face, scalp, arms)
- Considered a precancerous lesion that may develop into squamous cell carcinoma
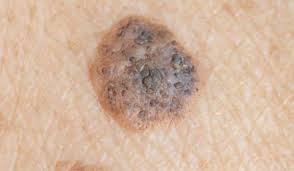
2. Seborrheic Keratosis
- Common, benign skin growth
- Appears as brown, black, or tan wart-like lesions
- Typically found on the chest, back, or face
- Not caused by sun exposure and not cancerous
3. Keratosis Pilaris
- Caused by keratin buildup in hair follicles
- Appears as tiny, rough bumps, often on the upper arms, thighs, or cheeks
- Harmless but may be cosmetically bothersome
What are the symptoms of Keratosis?
Symptoms vary by type, but may include:
- Rough or scaly skin patches
- Raised, crusty, or warty growths
- Skin discoloration (red, tan, brown, or black)
- Itching or irritation
- In keratosis pilaris: small bumps that feel like sandpaper
How is Keratosis diagnosed?
Diagnosis is usually clinical and may include:
- Skin examination by a dermatologist
- Dermatoscopy to inspect the lesion closely
- Skin biopsy – if there is suspicion of cancer or if the lesion changes in shape or color
How is Keratosis treated?
For Actinic Keratosis:
- Cryotherapy (freezing the lesion with liquid nitrogen)
- Topical creams – 5-fluorouracil, imiquimod, diclofenac
- Photodynamic therapy
- Laser or chemical peels
For Seborrheic Keratosis:
- Usually no treatment needed
- Can be removed for cosmetic reasons via:
- Cryotherapy
- Curettage
- Electrosurgery
- Laser therapy
For Keratosis Pilaris:
- Moisturizers with urea, lactic acid, or salicylic acid
- Gentle exfoliation
- Topical retinoids in persistent cases
- Regular skin care and avoiding harsh soaps
What is the prognosis for Keratosis?
- Seborrheic and keratosis pilaris are benign and not dangerous
- Actinic keratosis can potentially develop into skin cancer if not treated
- Most forms are manageable with regular skin care or minor procedures
Can Keratosis be prevented?
Yes, especially for types caused by sun exposure:
- Avoid excessive sun exposure
- Use broad-spectrum sunscreen regularly
- Wear protective clothing outdoors
- Moisturize daily, especially for dry or sensitive skin
- Get regular skin checks to monitor for new or changing lesions


