What is Juvenile Myositis?
Juvenile Myositis is a rare autoimmune disease in children that causes chronic inflammation of the muscles, particularly those closest to the trunk of the body, such as the hips, thighs, shoulders, and upper arms. This condition makes it difficult for affected children to perform daily tasks like climbing stairs, lifting objects, or even walking.
There are two main types:
- Juvenile Dermatomyositis (JDM) – the most common form, which includes a skin rash
- Juvenile Polymyositis (JPM) – rare and involves muscle inflammation without a rash
What causes it?
The exact cause is unknown, but it’s thought to involve an autoimmune reaction—where the body’s immune system mistakenly attacks healthy muscle tissues. Genetic predisposition and environmental triggers, such as infections or sun exposure, may contribute.
What are the signs and symptoms?
Symptoms often develop gradually and can vary in severity. Common signs include:
- Muscle weakness, especially in the hips, thighs, shoulders, and neck
- Fatigue and difficulty with physical activities
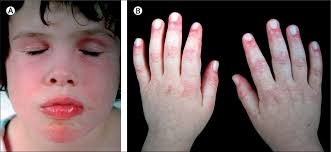
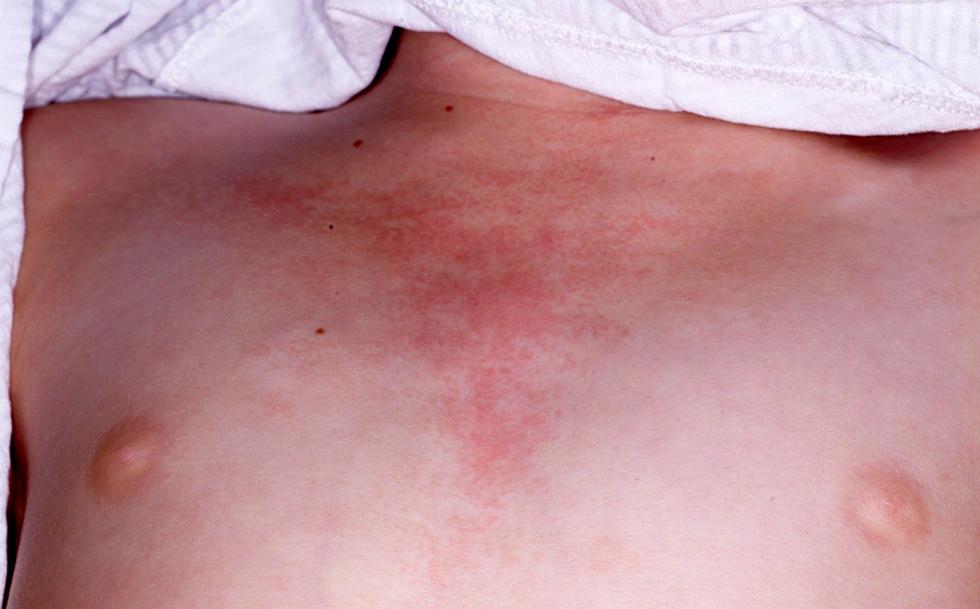
- Skin rash (in JDM) – often purple or red, found on the eyelids, knuckles, elbows, knees, or face
- Swelling around the eyes or face
- Calcium deposits under the skin (calcinosis) in some cases
- Muscle pain or tenderness
- Weight loss or poor growth
- Difficulty swallowing or breathing (in severe cases)
How is it diagnosed?
Diagnosis typically involves:
- Medical history and physical exam
- Blood tests, including:
- Elevated muscle enzymes (e.g., CK, LDH, ALT, AST)
- Autoantibodies (e.g., ANA, anti-Mi-2)
- MRI or ultrasound of muscles to detect inflammation
- Electromyography (EMG) to test muscle function
- Muscle biopsy (in some cases) to confirm diagnosis
- Skin biopsy (if rash is present)
How is it treated?
Treatment aims to reduce inflammation, improve muscle strength, and prevent complications. It often includes:
- Corticosteroids (e.g., prednisone) to reduce inflammation
- Immunosuppressive drugs (e.g., methotrexate, azathioprine)
- Biologic therapies (e.g., IVIG or rituximab) for resistant cases
- Physical therapy to maintain strength and flexibility
- Skin protection (in JDM) with sunscreen and clothing
- Calcium and vitamin D supplements if needed
What complications can occur?
If not treated properly, Juvenile Myositis can lead to:
- Severe muscle weakness
- Calcinosis (calcium deposits in skin or muscles)
- Joint contractures
- Swallowing or breathing problems
- Chronic pain or fatigue
- Delayed growth and development
Early intervention reduces the risk of long-term damage.
What is the outlook?
The prognosis varies. With early and effective treatment, many children recover well and regain normal muscle function. Some may experience flares or relapses, requiring ongoing management. Lifelong remission is possible in some cases, especially with Juvenile Dermatomyositis.
When should I see a doctor?
Contact a pediatrician or rheumatologist if your child has:
- Ongoing muscle weakness
- Unexplained skin rash
- Unusual fatigue
- Trouble with mobility or daily activities
Early diagnosis leads to better outcomes.


