What is Juvenile Polyposis Syndrome?
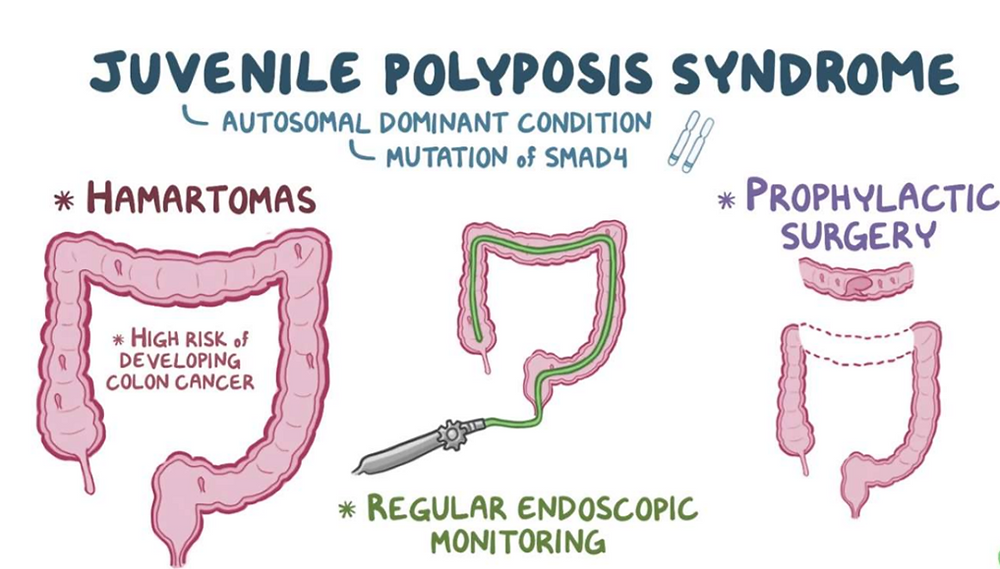
Juvenile Polyposis Syndrome (JPS) is a rare genetic disorder characterized by the growth of multiple noncancerous (benign) polyps in the gastrointestinal (GI) tract, especially the colon, rectum, and sometimes the stomach or small intestine. The term “juvenile” refers to the type of polyp, not the age of onset, although the condition typically appears in childhood or adolescence.
While the polyps themselves are benign, people with JPS have an increased risk of developing gastrointestinal cancers, particularly colorectal cancer.
What causes Juvenile Polyposis Syndrome?
JPS is primarily caused by inherited genetic mutations. It is most commonly associated with mutations in the following genes:
- SMAD4
- BMPR1A
These genes are involved in cell growth regulation, and mutations can lead to uncontrolled polyp formation. The condition follows an autosomal dominant inheritance pattern, meaning a person only needs to inherit one copy of the mutated gene from one parent to be affected.
In some cases, the mutation can occur spontaneously (without a family history).
What are the symptoms?
Symptoms may vary based on the number, size, and location of the polyps, but common signs and symptoms include:
- Rectal bleeding
- Anemia (due to blood loss)
- Abdominal pain or cramping
- Diarrhea or constipation
- Visible blood in the stool
- Prolapse of a polyp through the rectum
- In some cases, delayed growth or weight loss in children
Some individuals may have no symptoms and the condition is only found during routine screening or after complications arise.
How is Juvenile Polyposis Syndrome diagnosed?
Diagnosis involves a combination of clinical findings, imaging, and genetic testing:
- Colonoscopy or upper endoscopy – to visualize and biopsy polyps
- Polyp biopsy – to determine polyp type (juvenile-type polyps)
- Family history – important for assessing genetic risk
- Genetic testing – to confirm mutations in SMAD4 or BMPR1A
- Imaging tests – such as MRI or CT scans may be used to assess the extent of polyp growth
Diagnostic criteria usually include:
- More than 5 juvenile polyps in the colon or rectum
- Multiple juvenile polyps throughout the GI tract
- Any number of juvenile polyps in someone with a positive family history
How is Juvenile Polyposis Syndrome treated?
Management focuses on polyp removal, cancer prevention, and monitoring for complications:
Polyp Removal:
- Endoscopic polypectomy – during colonoscopy or upper endoscopy
- Surgery may be required in severe cases where polyp burden is high or cancer risk is significant
Surveillance:
- Regular colonoscopies and upper endoscopies starting in childhood or early teens
- Monitoring frequency depends on polyp growth and family history
Genetic Counseling:
- Offered to patients and families for risk assessment
- Relatives may be tested to determine if they carry the gene mutation
Cancer Risk Management:
- Some individuals may need prophylactic surgery, such as colectomy (removal of part or all of the colon), if cancer risk becomes too high
What is the prognosis?
With regular monitoring and early treatment, individuals with JPS can live long, healthy lives. However, the risk of colorectal cancer is significantly increased — estimated between 9% to 50%, depending on mutation and polyp burden.
Early diagnosis, lifelong surveillance, and proactive management are key to reducing cancer risk and improving outcomes.
Key facts to remember
- JPS is a genetic disorder leading to multiple benign GI polyps
- It is most often caused by SMAD4 or BMPR1A mutations
- Symptoms include rectal bleeding, anemia, and GI issues
- Diagnosed through endoscopy, biopsy, and genetic testing
- Requires regular monitoring and sometimes surgical intervention
- Carries a higher risk of colorectal cancer but is manageable with early care


