What is Juvenile Arthritis?
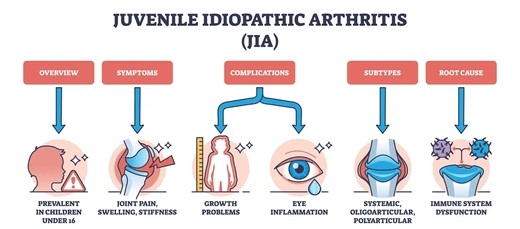
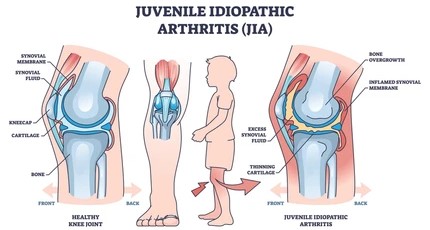
Juvenile Arthritis (JA) is a term used to describe inflammatory joint diseases that affect children under the age of 16. It is not a single condition but a group of autoimmune and inflammatory diseases that cause joint swelling, pain, stiffness, and reduced mobility.
The most common type is Juvenile Idiopathic Arthritis (JIA), formerly known as juvenile rheumatoid arthritis. JA can affect one or more joints and may also involve other parts of the body like the eyes and skin.
What causes Juvenile Arthritis?
The exact cause of Juvenile Arthritis is unknown, but it is believed to be an autoimmune disorder, meaning the immune system mistakenly attacks the body’s own healthy tissues, especially the joints.
While it is not directly inherited, genetic and environmental factors may play a role in triggering the disease.
What are the types of Juvenile Arthritis?
There are several types of JA, including:
- Oligoarticular JIA – affects 1 to 4 joints (most common and usually milder)
- Polyarticular JIA – affects 5 or more joints, often symmetrical
- Systemic JIA (Still’s disease) – affects joints and causes systemic symptoms like fever and rash
- Enthesitis-related arthritis – involves joints and areas where tendons attach to bones
- Psoriatic arthritis – occurs with psoriasis, a skin condition
- Undifferentiated arthritis – doesn’t fit into a specific category
What are the symptoms?
Symptoms of Juvenile Arthritis vary depending on the type but often include:
- Joint pain or tenderness
- Swelling and stiffness, especially in the morning or after rest
- Limited movement or limping
- Fatigue and irritability
- Fever and rash (especially in systemic JIA)
- Eye inflammation (uveitis), often without obvious eye symptoms
- Growth problems if untreated
Symptoms may come and go, with periods of flare-ups and remission.
How is Juvenile Arthritis diagnosed?
There is no single test to confirm Juvenile Arthritis. Diagnosis is based on:
- Detailed physical examination and symptom history
- Blood tests, including:
- Antinuclear antibody (ANA)
- Rheumatoid factor (RF)
- Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP)
- X-rays or MRI scans – to detect joint damage or inflammation
- Eye exams – to check for uveitis
- Ruling out other causes like infections or other autoimmune diseases
A diagnosis is made when symptoms persist for six weeks or longer in children under 16.
How is Juvenile Arthritis treated?
The goal of treatment is to reduce inflammation, relieve pain, and preserve joint function. Treatment may include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) – like ibuprofen or naproxen
- Disease-modifying antirheumatic drugs (DMARDs) – such as methotrexate
- Biologic agents – like etanercept or adalimumab for severe cases
- Corticosteroids – for flares or eye inflammation
- Physical and occupational therapy – to maintain mobility and strength
- Regular eye exams – especially for children with ANA-positive JIA
Early and aggressive treatment can significantly improve long-term outcomes.
What is the outlook for children with Juvenile Arthritis?
With proper treatment and follow-up, many children with Juvenile Arthritis lead full and active lives. Some may go into complete remission, while others may experience symptoms into adulthood.
Early diagnosis, tailored treatment plans, and supportive therapies are key to minimizing long-term joint damage and maintaining a good quality of life.
Key facts to remember
- Juvenile Arthritis is an umbrella term for autoimmune joint diseases in children under 16
- Symptoms include joint pain, swelling, stiffness, and fatigue
- Several subtypes exist, including systemic and psoriatic forms
- Treatment includes NSAIDs, DMARDs, biologics, and physical therapy
- Early treatment improves outcomes and helps children stay active and healthy


