What Is Eosinophilic Pneumonia?
Eosinophilic pneumonia is a rare lung condition characterized by an elevated number of eosinophils (a type of white blood cell) in the lungs. Eosinophils are usually involved in allergic reactions and immune responses to infections. In eosinophilic pneumonia, the buildup of these cells leads to inflammation and damage in the lung tissues, which can cause breathing difficulties and other respiratory issues. It is typically categorized into two types: chronic and acute eosinophilic pneumonia, each with varying severity and symptoms.
What Causes Eosinophilic Pneumonia?
The exact cause of eosinophilic pneumonia is not always clear, but it is often associated with several triggers:
- Infections – Certain parasitic, fungal, or bacterial infections can provoke an immune response leading to eosinophil accumulation in the lungs.
- Allergic reactions – Eosinophilic pneumonia can be triggered by allergies to inhaled substances like pollen, mold, or animal dander.
- Medications – Certain drugs, such as antibiotics, nonsteroidal anti-inflammatory drugs (NSAIDs), and chemotherapy medications, can sometimes cause an eosinophilic reaction in the lungs.
- Autoimmune disorders – Conditions like vasculitis and other autoimmune diseases may also contribute to the development of eosinophilic pneumonia.
- Environmental factors – Exposure to certain chemicals or inhalants in the workplace or at home, including dust or fumes, may trigger the condition.
What Are the Symptoms of Eosinophilic Pneumonia?
The symptoms of eosinophilic pneumonia can vary widely, depending on the severity of the condition. Common symptoms include:
- Shortness of breath – Difficulty breathing, especially during physical activity, is one of the hallmark symptoms.
- Coughing – Persistent coughing, which may be dry or produce mucus.
- Chest pain – Discomfort or pain in the chest due to lung inflammation.
- Fever – A mild to moderate fever often accompanies the condition.
- Fatigue – Many individuals with eosinophilic pneumonia experience extreme tiredness or weakness.
- Wheezing – Difficulty breathing with a wheezing sound, especially during exhalation.
In severe cases, symptoms can progress rapidly, requiring emergency medical intervention.
How Is Eosinophilic Pneumonia Diagnosed?
Diagnosing eosinophilic pneumonia involves several steps to rule out other potential causes of the symptoms. Key diagnostic methods include:
- Physical examination – A doctor will listen to the lungs for signs of wheezing, crackling, or other abnormal sounds that indicate lung inflammation.
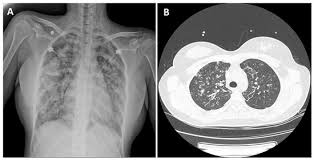
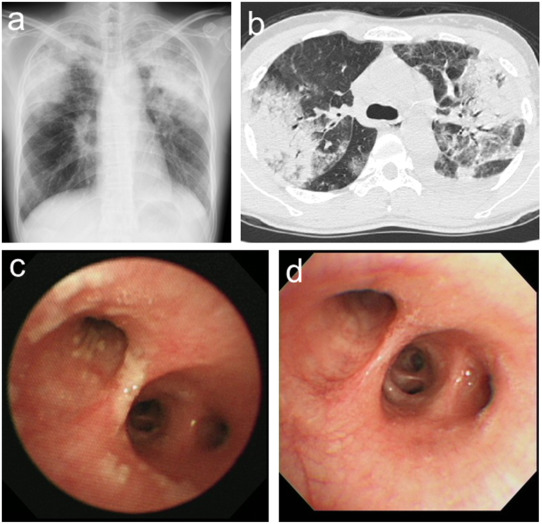
- Chest X-ray – A chest X-ray can show signs of lung inflammation, such as fluid accumulation or changes in lung tissue.
- CT scan – A more detailed imaging test that provides a clear picture of lung abnormalities.
- Blood tests – These may show an elevated eosinophil count, which is a common marker of eosinophilic pneumonia.
- Sputum culture – If the patient is coughing up sputum, testing the sputum can help identify any infections that might be contributing to the condition.
- Bronchoscopy – In some cases, a doctor may perform a bronchoscopy to collect samples of lung tissue or fluid to examine under a microscope.
What Is the Treatment for Eosinophilic Pneumonia?
Treatment for eosinophilic pneumonia depends on the severity of the condition and its underlying cause. Common treatment options include:
- Corticosteroids – The primary treatment for eosinophilic pneumonia is the use of corticosteroids (such as prednisone) to reduce inflammation and control eosinophil levels in the lungs.
- Oxygen therapy – In severe cases, oxygen therapy may be required to ensure that the body receives enough oxygen.
- Antibiotics or antifungal medication – If an infection is the underlying cause of the pneumonia, appropriate medications such as antibiotics or antifungals will be prescribed.
- Discontinuing triggering medications – If a medication is found to be causing the condition, stopping the medication may improve symptoms.
- Immunosuppressive drugs – In cases where the condition is not responding to corticosteroids, additional immunosuppressive treatments may be required.
- Supportive care – This includes staying hydrated, getting rest, and using other methods to support lung function while the condition resolves.
Can Eosinophilic Pneumonia Be Prevented?
Preventing eosinophilic pneumonia can be challenging, as it is often triggered by factors such as infections, allergies, and certain medications. However, some preventive measures can reduce the risk of developing this condition:
- Avoiding known allergens – If you have known allergies to certain substances (such as pollen or pet dander), avoiding exposure can help reduce your risk of triggering an allergic reaction that could lead to eosinophilic pneumonia.
- Taking medications as prescribed – If you are prescribed medications that could trigger an eosinophilic response, it’s essential to follow your doctor’s instructions carefully and report any unusual symptoms promptly.
- Protecting yourself from infections – Practicing good hygiene, getting vaccinated, and avoiding exposure to infectious agents can help prevent respiratory infections that might trigger eosinophilic pneumonia.
- Limiting exposure to environmental toxins – If you work in an environment with inhalants or chemicals that could irritate the lungs, take necessary precautions such as wearing protective gear.
What Is the Prognosis for Eosinophilic Pneumonia?
The prognosis for eosinophilic pneumonia can vary. In many cases, with early treatment, the condition improves significantly, and patients can make a full recovery. However, if left untreated, the inflammation can lead to lasting lung damage. Chronic cases of eosinophilic pneumonia may require long-term management, including ongoing corticosteroid use.
In general, the outlook is favorable for those who receive prompt treatment. Most individuals recover within a few weeks to months, although some may experience relapses or complications.
What Support Is Available for People with Eosinophilic Pneumonia?
Living with eosinophilic pneumonia can be challenging, especially if the condition is recurrent. Support resources available for patients include:
- Patient support groups – Many organizations offer support groups for people affected by rare respiratory conditions, providing emotional support and practical advice.
- Medical professionals – Regular visits to pulmonologists or other specialists can help manage symptoms and prevent flare-ups.
- Online communities – Online forums and communities can connect individuals with similar experiences, offering a space to share information and tips for managing the condition.
- Counseling and therapy – For individuals struggling with the emotional impact of chronic illness, therapy and counseling can provide valuable support.


