Overview
Artificial sweeteners—such as aspartame, sucralose, saccharin, acesulfame potassium, and stevia derivatives—are widely used in diet products, sugar-free foods, and beverages. While considered safe in moderation, growing research links these sweeteners to gastrointestinal (GI) disorders and gut microbiome disruption. Their non-nutritive, non-digestible nature can trigger adverse reactions in sensitive individuals and may contribute to long-term gut health issues.
Causes and Mechanisms
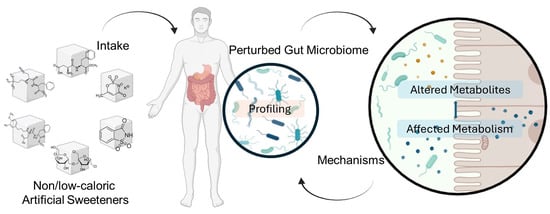
- Microbiome Disruption: Many artificial sweeteners alter the gut flora composition, reducing beneficial bacteria and promoting dysbiosis.
- Osmotic Effects: Some sweeteners like sorbitol and xylitol (sugar alcohols) draw water into the intestines, leading to diarrhea or bloating.
- Inflammatory Responses: Certain sweeteners may increase gut permeability and low-grade inflammation.
- Fermentation: Non-absorbed sweeteners are fermented by gut microbes, producing gas and discomfort.
- Individual Sensitivity: People with IBS or IBD may be particularly sensitive to even small amounts of artificial sweeteners.
Commonly Associated GI Disorders
- Irritable Bowel Syndrome (IBS)
- Functional Bloating and Gas
- Chronic Diarrhea or Constipation
- Small Intestinal Bacterial Overgrowth (SIBO)
- Food Intolerances and Sensitivities
- Increased Risk of Inflammatory Bowel Disease (emerging evidence)
Symptoms
- Bloating
- Flatulence
- Abdominal cramps
- Diarrhea or constipation
- Nausea or a sense of fullness
- Changes in bowel habits after consuming diet drinks or sugar-free products
Diagnosis
- Diet History: Key to identifying patterns linked to artificial sweetener intake.
- Elimination Diet: Temporary removal of sweeteners to observe symptom changes.
- Breath Tests: May be used to detect SIBO or fermentation byproducts.
- Stool Tests and Microbiome Analysis: Research tools to evaluate gut flora shifts.
Treatment and Management
- Elimination or Reduction: Removing artificial sweeteners from the diet often alleviates symptoms.
- Low-FODMAP Diet: May help individuals with IBS triggered by certain sugar substitutes.
- Probiotics and Prebiotics: To help restore gut microbial balance.
- Hydration and Fiber: Support digestion and regular bowel function.
- Medical Therapy: For underlying GI conditions (e.g., antispasmodics for IBS, antibiotics for SIBO).
Preventive Measures
- Read Food Labels: Identify and avoid artificial sweeteners in processed foods and beverages.
- Choose Natural Alternatives: Limit use of synthetic sweeteners; consider small amounts of natural sweeteners like honey or fruit-based options.
- Moderation is Key: Even “safe” sweeteners can cause trouble in high or frequent doses.
- Educate Vulnerable Populations: People with digestive disorders should be counseled on the potential GI impacts of artificial sweeteners.
Prognosis
For most individuals, symptoms resolve after reducing or eliminating artificial sweeteners. However, chronic gut microbiome disruption may have long-term health implications, including links to metabolic and inflammatory diseases.
Global Trends
- Increasing use of sugar substitutes in low-calorie products amid rising diabetes and obesity rates.
- A rise in GI complaints linked to dietary additives in high-income countries.
- Growing interest in the gut-brain axis and how sweeteners may impact mental and digestive health.


